The Hospital
As you may remember, I spent four days in my local hospital, during which I received an IV antibiotic (Tazocin), before being discharged on a seven day course of an oral antibiotic (Flucloxacillin), with the plan of having a check-up at the hospital in Sheffield a week later to see how I was getting on. At that check-up the doctor recommended that I arranged to see a podiatrist at my local health centre, so that a specialist could suggest what was the best way forward. However, it turned out that I needed to see my G.P., in order to get a referral to see a podiatrist, so I made an appointment.
The G.P.
When I saw my G.P., a week later on the 5th of November (day +278), I was given another seven day course of the same oral antibiotic, as well as a topical antibiotic (Mupirocin), and referred to see a podiatrist, as my big toes were looking infected again; Fortunately, the infection was only local this time, hence I mostly felt fine. It was really only because of my medical history that the G.P. referred me to see a podiatrist, and that I got an appointment relatively quickly, i.e. the 14th of November (day +287).
I actually spoke to my G.P. again a couple of days prior to the podiatrist appointment, as my big toes still looked infected, hence I needed some more of the oral antibiotic. Whilst picking-up my prescription from my local health centre, I went to see a nurse there too, so that a swab could be taken to send off to the microbiology department at a nearby hospital, in order to identify the specific infection that I had; Determining the specific infection helps with choosing the best antibiotic(s) to use to treat it.
The Podiatrist
After I'd explained my medical history, in particular my immuno-suppressed status, and shown my big toes to the podiatrist, we had a discussion about what was the best way forward. The podiatrist explained that my toenails were not so much ingrowing as slightly too wide - A common issue. In other words, the infection was resulting in my big toes becoming quite swollen, and that was making the toenails look ingrowing.
Essentially, I had two main options available to me: Continue with the antibiotics to clear-up the infection, and then either hope that they healed by themselves, or have some form of toenail surgery to help them heal. The toenail surgery would involve either removing the toenails, or just the edge(s) of the toenails so that they weren't quite so wide - An acid would then be used to prevent whatever was removed from ever growing back. Whilst the podiatrist seemed to be leaning towards some form of toenail surgery, it was made clear that the toenail surgery is unsuccessful in a small percentage of cases, and that whatever option I chose, there was a risk of my big toes becoming infected again; i.e. there was no right or wrong option really.
My immuno-suppressed status meant that any form of toenail surgery would need to be done by a surgeon in a hospital theatre, in order to minimise the risk of infection; Normally, the procedure would be done by the podiatrist at the local health centre. The hospital setting also meant that blood tests could be performed prior to the surgery to ensure that any potential issues with excessive bleeding could be prevented, and antibiotics could be given afterwards to hopefully prevent any issues with infection.
Fortunately, I didn't have to make any decision there and then, as the podiatrist was just going to write a letter to my G.P. to explain the situation, i.e. the G.P. would then contact me to discuss what to do next, and organise the toenail surgery if applicable. In the mean time, I'd continue with the antibiotics and wait for the results of the swab.
The Swab Results
The morning after visiting the podiatrist, the swab results were back, and the infection had been identified as Pseudomonas Aeruginosa. No doubt that clears it all up for you, but I had to turn to my trusty friend Google to see whether it had anything of interest to share with me. As if by magic, it guided me to a couple of articles, amongst which two particular sentences stood out: "In immunocompromised patients, systemic infections can occur which may be severe and associated with a high mortality." [1] and "While mortality from the infection varies depending on where the infection is, how soon it is treated and the underlying weakness of the patient, some studies suggest a third of infected patients may die." [2]. That knowledge really helped to set my mind at rest!
With my curiosity well and truly satisfied, I decided to watch an episode of Grey's Anatomy (an American medical drama). The episode in question happened to be a story about one of the show's doctors being sued by a professional snowboarder. The professional snowboarder had acquired a post-operative infection after having a hip replaced. That infection ultimately led to both legs needing to be amputated. Why do I mention it? I hear you say. Well, as coincidence would have it, the writers had decided that the infection was none other than Pseudomonas! For the rest of the episode, I couldn't help but laugh each time one of the characters mentioned its name!
The District Nurse
Amusing stories aside, my G.P. recommended that I continued with the antibiotics, and organised a district nurse to contact me, so that some silver dressings could be used to cover my big toes, in order to reduce the chances of them continually getting infected. In other words, it seemed like, whilst the current infection was limited to my big toes, it wasn't really of much concern, as the antibiotics would clear it up, and the silver dressings would reduce the chances of acquiring any further infections.
As it happened, there were a couple of days between talking to a district nurse, and actually seeing one, as inbetween was the weekend; i.e. that time of the week when medical conditions take a break from their normal chaos causing duties, so they can recharge their batteries ready for another week of madness. Once the weekend had passed, I hobbled my way into the district nurse's clinic, who helpfully covered my big toes with the silver dressings, whilst in the process demonstrating how I could do so myself, and provided me with the necessary supplies for redressing them each day.
Back to the Hospital
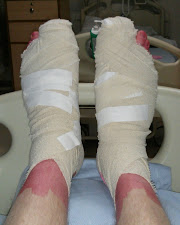
The day after seeing the district nurse, I'd once again completed the course of oral antibiotics, but my big toes still weren't really looking any better, so I asked what the hospital recommended doing next - I had been keeping the hospital, specifically one of the bone marrow transplant co-ordinators, up-to-date with what was happening, just in case the specialists there had any additional insight to offer, given my medical history, hence the hospital was aware of my situation. In fact, said bone marrow transplant co-ordinator was probably a bit too aware, as I'd kindly provided photos of my big toes, so that my progress (or lack thereof) could be clearly seen! No doubt you're now itching to see the photos yourself, so, for your viewing pleasure, I hereby present:
The hospital recommended that I made my way in, so that I could be seen by one of the doctors, and in all likelihood be admitted and started on an IV antibiotic (Tazocin). That was indeed exactly what happened, but I was also prescribed an oral antibiotic (Metronidazole), as I mentioned that I'd been going to the toilet much more frequently again, and, even though I wasn't at the diarrhea stage, it reminded me of my recent run-in with C. Diff, hence I wondered whether the recent courses of the previous oral antibiotic (Flucloxacillin) had resulted in me heading back down that road.
On admission, a whole bunch of swabs were taken, none of which actually identified anything, but the swabs of my big toes were repeated the next day (when they were oozing) and they did confirm the results of the swabs taken at my local health centre, i.e. the infection was Pseudomonas Aeruginosa. Therefore, the plan was to continue with the antibiotics until the weekend had passed (day +298), when I would then see a specialist about what (if any) toenail surgery was necessary to resolve the issue.
The Acute Trauma Surgeon
It was late on the Monday evening when an acute trauma surgeon came to see me. To be perfectly honest, both the nurses and myself were quite surprised to see someone at that time. However, it turned out that someone else needed to see me really, i.e. someone that specialises in feet, so the acute trauma surgeon arranged for that to take place the next day. Having said that, we did have a brief discussion about removing the toenails etc, which was similar to the one I'd had with the podiatrist.
The next morning, when the doctors were doing their daily rounds, the roles kind of reversed a bit as I had to update the doctors with what the acute trauma surgeon had said and done, as even though it had all been carefully documented in my medical notes, one of the doctors described the calligraphy as beautiful but illegible. At the same time, I mentioned that my heart rate was still a bit high, and I was continuing to find myself a bit out-of-breath on light activity. The result of which was that the doctors arranged for me to have an electrocardiogram and echocardiogram later that day, just in case they shed any light on the subject - The results of both turned-out to be fine.
The Mystery Guest!
I'm told the specialist arranged by the acute trauma surgeon did come to see me, but unfortunately it was whilst I was having the echocardiogram, hence that meant waiting another day for the specialist to return. However, for whatever reason, the specialist never turned-up the next day, but I was assured that the specialist would come to see me the day after. The day after, someone did actually come to see me, and, whilst that person didn't quite look like what I was expecting, I assumed it was the specialist.
We had a chat about my big toes, which once again went along similar lines to the one that I had with the podiatrist, and the result was that I could go home on a different oral antibiotic, i.e. one that would hopefully clear-up the infection, with the plan of perhaps having some form of toenail surgery at a later date. I was keen to make my escape by this point, as the previous day I'd been moved to a different ward, which for various reasons is not as nice, hence I bugged the poor nurse that was looking after me to chase the doctors to arrange my discharge. If you are wondering why I'd been moved, it was due to a shortage of beds and that other patients were more ill than myself.
Later that day, one of the doctors came to see me, and started to apologise that the specialist (who is based at a nearby hospital) had once again not turned-up, and to address this issue arrangements had been made for me to go and see the specialist instead, as that would make it easier for us both to be in the same place at the same time. As you might imagine, I was somewhat confused, as I thought I was about to get discharged! After explaining the confused look on my face, and the doctor going to see what the mystery guest had written in my medical notes, it turned-out that no-one was quite sure who had come to see me, but it didn't matter as I needed to see someone more senior, i.e. the specialist (an orthopedic surgeon). Unfortunately, that meant it was more like my plans that would be escaping out of the window than myself.
Later that evening, after I'd remade the bed from the sheets I'd carefully tied together to lower me to my escape, another doctor came to see me (someone more senior). The doctor wanted to explain that behind the scenes a number of discussions had been going on (at various levels) to try to get things sorted, but a few issues were making it quite complicated: It's hard for the different specialties to fully appreciate my medical history; the particular infection I had, when combined with my recent run-in with C. Diff, meant that there wasn't really any good options for oral antibiotics; and communication and organisation can be tricky when different hospitals and departments are involved. That all meant that I might need to push a bit to get things done in a timely fashion.
The Orthopedic Surgeon
The next day, the hospital arranged transport for me to see the orthopedic surgeon. Due to the transport being arranged at the last minute, I had to go and return by taxi. Fortunately, that meant I didn't need to rely on the normal hospital transport, which is infamous for its waiting times, and that a member of the medical staff would need to go with me, as only they are allowed to take my medical notes. Whilst that may seem like a waste of NHS resources, if you ever saw the size of my medical notes, you'd soon realise that it takes someone that is both fit and healthy just to lift them!
Surprisingly, we had only been sat in the waiting area for a few minutes, before we were called in to see the orthopedic surgeon. Once again, I found myself discussing my big toes, and much like with all of the prior discussions, they didn't seem to be of much concern, as the orthopedic surgeon recommended that I was discharged on oral antibiotics, and I had another appointment in a month or so to decide what exactly was next. That recommendation was at the opposite end of the scale to what the senior doctor (consultant) had said would be best the previous evening. I had tried to explain that to the orthopedic surgeon, but I probably could have done so much more clearly, if I'm honest; I was just a bit taken aback by the difference in opinions.
As you might imagine, I was also kind of between a rock and a hard place, as I had two highly qualified and experienced medical professionals, albeit in very different specialties, recommending quite different treatment plans; I was just the lay person in the middle trying my best to not sound like some kind of crazed hypocondriac - I can't help but think that the orthopedic surgeon would likely say that I was unsuccessful!
As we made our way back in the taxi, I was thinking everything through, and could see how the consultant would likely not be very happy with the plan recommended by the orthopedic surgeon, so given that the nurse that worked with the orthopedic surgeon had given me a phone number that I could use to get in touch, I thought I'd give the nurse a quick call to make sure I'd understand what had been said, and that I'd clearly explained the issues around my medical history etc. As it happened, the nurse was unavailable when I called, so I arranged to call back a bit later, but not long afterwards the nurse actually called me, and we had a quick chat, before the nurse offered to put the orthopedic surgeon on the phone. After a chat with the orthopedic surgeon, where it seemed like I made a much better job of explaining things, another appointment was arranged for after the weekend, so that we could once again discuss what was best.
Foiling my own Escape!
Shortly after talking to the orthopedic surgeon on the phone, one of the doctors came to tell me that my discharge was being arranged, as recommended by the orthopedic surgeon, and that I'd go home on some form of oral antibiotic(s), i.e. a concoction that would hopefully cure the infection and not result in the C. Diff returning. However, after I explained that I'd just spoken to the orthopedic surgeon again, and that I now had another appointment after the weekend, my discharge was cancelled yet again.
Amusingly, as I was talking to the doctor, I found myself a bit distracted by one of the other doctors clearly struggling to find the meeting point between the curtains that had been pulled around my bed for privacy; I couldn't help but smile really, as the doctor in question had not particularly inspired me with confidence on prior occasions, hence being outwitted by a pair of curtains was kind of the final nail in that coffin, so to speak. It only amused me further when yet another doctor later joined the discussion, without even the slightest hint of any difficulty finding where the two curtains met.
Back to the Orthopedic Surgeon
Once the weekend was over, I was on my way back to see the orthopedic surgeon. Once again, a member of the medical staff and myself were going and returning by taxi, as it had been arranged at the last minute; I'd not chased organising it, as it clearly wasn't in my interest to do so. We did have to wait a bit before seeing the orthopedic surgeon, but I hardly had to say a word when we did, as the plan was now to remove the toenails on both of my big toes on the 9th of December (day +312), which in case you have lost track was only a week away. The plan wasn't a cast iron certainty though, as it sounded like some schedule juggling would be necessary.
Essentially, after a few quick questions about the likelihood of the surgery being successful, and the probability of getting an infection, I really just had to sign the consent form, and go to the pre-operative assessment clinic, where they would do a few routine tests to ensure that I was ready for the surgery. The surgery is successful in about ninety-five percent of cases, i.e. in the others part of the toenail grows back and may require further surgery. However, putting a number on the risk of infection wasn't really possible for me, due to my medical history; Normally, only about one or two percent of cases have an issue with an infection, but that was a bit academic.
There was another topic that was briefly discussed, and that was whether it was worth having an x-ray or MRI of my feet to see if the infection had spread to my bones, as that would mean changing the treatment plans somewhat. This had originally been queried by someone in the orthopedic team, but it seemed everyone thought it was extremely unlikely, even with my medical history. It was mentioned that an x-ray isn't really clear enough to say one way or the other though, so it would need to be an MRI if it was felt necessary. Also, should the MRI show that the infection had spread to my bones, the procedure would likely change to amputating my big toes instead. After the latter comment, I soon agreed to give just removing the toenails a try first!
The Receptionist
We had to wait a bit before we could make our way to the pre-operative assessment clinic, as one of the nurses needed to check whether they could squeeze us into their schedule - Ideally, as soon as possible, as we needed to get back to the other hospital really. The nurse went to see what could be done, but soon returned to say that in fifteen minutes it would be necessary to call them about it, as the person required was on a break. The nurse was actually going for a break now too, so the message was passed on to another nurse. That nurse said I'll just go again in a few minutes. The response to which was: You are brave. Despite that, the nurse went anyway.
At the time, we didn't really understand the comment about being brave, but it wasn't long after we were pointed in the direction of the pre-operative assessment clinic that it started to become clear, as everyone in the queue at the reception desk felt like they had been put in the naughty corner when they were asked to take a few steps back to wait in the designated area. To be honest, it was fair enough really, as the rationale was to give at least the illusion of privacy to the patient at the reception desk. After that, we definitely weren't going to leave the designated area until we were called though!
When we were called, we cautiously took the few steps forward to the reception desk, each of us wondering who was going to be the brave one that explained why we were there - It turned-out, it was the member of the medical staff that had come with me. After explaining that we were hoping to be squeezed-in as soon as possible, so that I could get back to continue my course of IV antibiotics, we were asked to take a seat whilst someone checked what (if anything) could be done. It was only a few minutes later that we were told that because I was going to have the toenail surgery with just local anaesthesia, we didn't need to see someone in the pre-operative assessment clinic, as the ward where I was admitted had likely done all of the necessary tests, and even if any other tests were required, they could easily be done on the ward. That just left building-up the courage to ask the receptionist about booking the taxi back.
The receptionist called the number that we provided for the taxi, but was asked to try again in half an hour when someone would be back from lunch. In the mean time, we were told to take a seat. That sounded a bit strange, but we didn't dare to question it. A little over twenty minutes later I asked the receptionist about trying again, but, after the receptionist had checked the time, I was told we needed to wait another ten minutes, so I sheepishly headed back to my seat - That told me! It was about fifteen minutes later when the taxi was booked though, after which we were soon on our way back.
Should I stay or Should I go?
That same day, the doctors decided to reduce my Ciclosporin dose from 100mg/day (50mg in the morning and at night) to 75mg/day (50mg in the morning and 25mg at night), as that would reduce my immune suppression slightly, thereby hopefully putting me in a better position to recover from and avoid further infections. Also, because the blood sample that had been taken several weeks earlier for checking my chimerism seemed to have just vanished, I needed to have another chimerism blood test - When the results came back, they showed that I was still 98% donor (full chimerism).
The next day, one of the doctors informed me that I was being discharged, and that I would go home on some concoction of oral antibiotics, which would hopefully keep me heading in the right direction, and that I would need to return a few hours before my toenail surgery for a couple of platelet transfusions, in order to prevent excessive bleeding. However, shortly afterwards it occurred to me that my blood counts had perhaps not been checked in preparation for my ECP treatment over the next two days. When one of the doctors checked, it turned-out that my hemoglobin was a bit low, hence that meant I needed a couple of red blood cell transfusions, therefore I'd be around for several more hours whilst they were ordered and pumped into me.
Whilst waiting, another doctor (someone more senior) stopped by to say that, after a discussion with the orthopedic surgeon, it seemed that in all likelihood my discharge would be cancelled; I likely needed to stay on the IV antibiotic, as there was some concern that the concoction of oral antibiotics wouldn't suffice, which would prove problematic for the toenail surgery. Either way, someone would let me know.
Later that day, yet another doctor told me that I could go home, as originally planned, if that's what I wanted to do. Inbetween, I'd seen a number of nurses etc too; Some of whom thought I was staying, and some of whom thought I was going. I'm pretty sure that the medical staff must have thought that I'd completely lost the plot, as I was never really sure whether I was staying or going, as it was difficult to tell who had the most up-to-date information about what was happening. In the end, I decided to stay for at least another couple of days, as: it was going to be late by the time the red blood cell transfusions finished; the next two days I needed to go to a nearby hospital for my ECP treatment; and there seemed to be some uncertainty around the concoction of oral antibiotics, so staying on the IV antibiotic was likely the better treatment.
Two days later, the decision about whether to go home for a few days was pretty much made for me, as it wasn't long now before the toenail surgery, so it seemed kind of pointless risking the concoction of oral antibiotics for the sake of a bit of time at home. The IV antibiotic was clearly working, slowly but surely, so continuing with it was still the better treatment plan really, and could potentially prevent any further issues.
Amusingly, the same day, my G.P. phoned me to say that the podiatrist's letter had arrived, and I needed to decide whether I wanted to go ahead with the toenail surgery. I was a bit surprised by the call, as I had mentioned to the G.P.'s secretary (a little over two weeks earlier) that I was almost certainly being admitted into hospital to get things sorted, but nevertheless I: explained that everything had already been arranged, apologised for the apparent lack of communication, and said thanks for the call.
Passing the time!
The only problem with choosing to stay in hospital (putting aside the delightful cuisine) is that there isn't a great deal to do. Inbetween getting showered, eating meals, taking medications, checking observations and the doctors' rounds, I mostly killed a few brain cells watching TV and tormented myself reading my Facebook news feed etc. Having said that, for reasons that are probably best left unexplained, Christmas decorations was a hot topic on the ward at the time, so one evening I distracted myself for a bit by making an intricate looking paper snowflake. Another evening I decided to do some more drawing; Specifically, Minnie Mouse as a nurse. You can check-out both of my creations below - As usual, simply click on the images to view them full size:
The Unexpected
As I mentioned earlier, I needed a couple of platelet transfusions before the toenail surgery, and it turned-out that the kind donor(s) had shared almost double the normal volume, which made the timing tight, so they were transfused (one after the other) at the maximum rate that the IV pump could handle. Whilst I'd never had problems with platelet transfusions in the past, it seemed like the combined volume and rate proved a bit too much for me, as I had a slight reaction to them; I was itchy and a hive like rash appeared. An antihistamine (Piriton) soon resolved that issue for me though.
After I'd been transported to the nearby hospital where the toenail surgery would take place, I had a surprise visit from a member of the physiotherapy team, as it turned-out that I needed crutches after the toenail surgery, as I'd likely struggle with walking for a bit, given both of my big toes were being operated on. The crutches were adjusted to suit my height, and I was shown how to walk with them, as well as how to go up and down stairs. I was also given a leaflet on the subject to help jog my memory.
The Toenail Surgery
It had been a long time coming, but the weekend had passed, and it was finally time for the toenail surgery. By this point, the IV antibiotic (Tazocin) had enabled both of my big toes to look and feel almost normal again, hence it was a bit disappointing in a way that I was now about to make them pretty sore for a while. However, had I even jokingly suggested the idea of not bothering with the toenail surgery, I think my doctors would have almost certainly suffocated me with a pillow, so in the grand scheme of things sacrificing a couple of my toenails was clearly the wisest choice that I could make.
Whilst you may actually prefer to take my word for how the IV antibiotic (Tazocin) proved to be superior to the oral antibiotic (Flucloxacillin) for clearing-up the infection (Pseudomonas Aeruginosa) in my big toes, I thoughtfully kept track of my progress with another set of photos, so you didn't miss out on the oozing of blood and pus - I actually took them to enable the doctors to see the progress, as the vast majority of the time my big toes were covered with dressings to help keep them clean, but...
It wasn't long before it was time for the orthopedic surgeon to start the ball rolling, which meant injecting the local anesthetic into both of my big toes. This was the bit that I was least looking forward to, as in the words of the orthopedic surgeon "it will smart a bit" and "it will hurt you more than it hurts me". The needle was almost long enough to go right through my big toes, and it needed to be gradually pushed all of the way in, whilst injecting the local anesthetic, in a couple of places in both big toes.
As the orthopedic surgeon started to inject the local anesthetic, you could see the medical staff looking at me with great anticipation of a mixture of profanities and screaming, whilst at the same time thinking to themselves "wait for it... wait for it...", but much to my relief (and perhaps disappointment of everyone else) I hardly felt a thing. That meant, after giving it a few minutes to kick-in, whilst the orthopedic surgeon etc dressed for theatre, it was time to wish a final farewell to a couple of my toenails.
As I was pushed into the theatre on an operating bed, I remember thinking that all of the gadgets made it look pretty impressive, but perhaps more memorably I decided to comment that the medical team (in their surgical gowns) looked like the teletubbies. After hearing those words leave my mouth, I added that was probably not the best thing to say to the highly-skilled medical professionals that are about to take a scalpel to your big toes. Fortunately, only the person pushing the operating bed heard me!
The operation itself seemed pretty simple. I could actually watch the orthopedic surgeon work on one of my big toes, whilst someone else was guided through the process of doing the same to my other. The only slight complication was that I needed a bit more local anesthetic in one of my big toes, as I could still feel it at first. It did seem to surprise at least one member of the medical staff that I watched it all.
Essentially, after checking that the local anesthetic was working and tourniquets had been applied to stop my blood gushing out, the toenails could pretty much just be pulled off. That left using a scalpel to make a few incisions along the bottom of where the toenail had been, applying some acid (Phenol) to the same area to prevent the toenail from coming back, thoroughly washing the acid away with saline after about forty-five seconds, putting a dissolvable stitch at the bottom of each side of where the toenail had been, applying a sufficient amount of the pressure dressing to remove the tourniquets, removing the tourniquets, and completing the pressure dressing. (I've glossed over the various cold fluids applied to my feet to help prevent infection.)
Once the toenail surgery had been completed, I had to slide my way on to a hospital bed, so that I could be taken to another room for an hour or so, where my observations could be checked regularly, before being transported back to my hospital of origin. It all went smoothly, except that as I climbed my way out of a wheelchair into bed, thereby completing my journey, I realised that my shiny new crutches had been lost in transit. All was not lost though, as I did still have the leaflet describing how to use them!
The Aftermath
Unsurprisingly, after having your feet operated on, it is recommended that you keep them elevated to prevent excessive bleeding. The plan was for me to spend a couple more days on the IV antibiotic, before being discharged on the concoction of oral antibiotics, hence keeping my feet elevated was easy enough. The reason for staying that bit longer in hospital was to hopefully prevent my big toes from getting infected.
Unfortunately, despite my feet being elevated, later that evening (and through-out the night) they bled quite a bit. The nurses that were looking after me had to clean-up the blood that was all over the end of my bed and the floor on a few occasions. I also saw a couple of different doctors, as it wasn't something that any of the team there had encountered previously, hence they wanted to ensure that I got the right treatment.
Initially, some additional dressings were added over the top of the existing dressings, in order to help stop the bleeding, but later on those dressings were removed, as well as part of the original dressing on one foot, as they were all soaked with blood. After adding more dressings to replace those removed, the bleeding eventually stopped. However, over the next day or two, as the blood dried-up, the dressings on my feet turned into what felt like concrete boots, which ended-up being pretty uncomfortable!
It was actually the concrete like boots that resulted in yet another discharge being cancelled; I'd asked whether the dressings could be replaced, as I didn't want to go home with them squashing and digging into my feet, unless I really had to do so. However, that meant waiting another day, so that the right people could be asked about removing the dressings, and what exactly would need to be put on in their place.
Home Sweet Home!
The next day, one of the nurses had managed to contact someone to check about replacing the dressings, and I could finally get rid of my concrete like boots, and head on home! The poor nurse that acquired the job of replacing the dressings proved to have quite the challenge on her hands though, as with all the dried-up blood, they weren't coming off easy. I had to soak my feet in hot water on a couple of occasions, as parts of the dressings were removed, and removing the last bits around my big toes themselves wasn't the most pleasant of experiences, as it sure stung a bit!
Both the nurse and myself had hoped that once the dressings were off, it would just be a relatively simple job of applying some new dressings, and I'd be ready for going home. However, removing the dressings resulted in yet more bleeding, particularly on one of my big toes. The nurse tried applying pressure and using a tranexamic acid solution (it helps blood clot), but still had to replace the dressings a couple more times during that morning before the bleeding actually stopped. Even the dressings that I finally went home with looked a bit red, but they were much more comfortable, so I could live with that until they were redressed, as it was only the next morning that I had an appointment at the dressings clinic to get them checked and redressed yet again!
On the 12th of December (day +315), I actually made it all of the way through the discharge process, and went home with my usual medications, some tranexamic acid tablets, and the concoction of oral antibiotics that would hopefully keep me infection free. The concoction turned-out to be Ciprofloxacin, for mopping-up any remaining Pseudomonas Aeruginosa, and Vancomycin, for preventing C. Diff from returning.
Note: I had wondered whether I might be prescribed Vancomycin, as that's what I was given when I actually had C. Diff; My thinking was that if it could be used to treat it, then perhaps it could be used to prevent it too - The doctors didn't seem sure either though, as it's not something they'd normally do. (As it turned-out, the week of Ciprofloxacin and Vancomycin slowly pushed my stools in the direction of diarrhea, but the extra week of Vancomycin afterwards brought things back again. That likely means I made the right decision to stay in hospital on the IV antibiotic prior to the toenail surgery, as I'd imagine that two weeks of Ciprofloxacin would have proven problematic.)
The next morning, the dressings were still a bit awkward to get off, but nowhere near as bad as the previous day. Even though the nurse redressed them slightly differently, my feet still looked like something out of "The Mummy"! It wasn't actually until five days later when they were redressed again that the dressings were scaled-down a lot. You can see what the dressings immediately after the toenail surgery, and the dressings once scaled-down, look like below - I'm saving what lies beneath for another post:
The Lesson Learnt
I've previously joked that, after being diagnosed with cancer, you need to talk to the hospital that managed your care about any health issues, because your medical history complicates nearly everything; Your G.P. can only help with something as trivial and clearly unrelated as an ingrowing toenail! Well, after the above experience, which still may not even be over, it seems I need to find myself a better example!