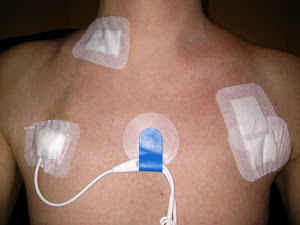
As it happens, my timing of this post is not ideal, as I need to start by contradicting myself a little. Due to my recent toenail surgery, hickman line replacement, and skin GVHD issues, I do actually have more visible on the surface than usual, so even the least observant amongst you would likely notice something. However, the first two will shortly be not so easy to spot (given sufficient time to heal), and the dry, flaky, red skin caused by the last (should it not be cured) might easily be mistaken for soaking-up too many of the sun's rays. Having said that, if you were to put your detective hat on, and look at me closely, there are a few things that you couldn't dismiss as normal:
-
Scars - There are several very minor scars, which are only just visible upon close inspection, as a result of having a number of bone marrow and skin biopsies, and hickman line insertions and removals.
-
Tattoos - There are a few tiny tattoos, which are simply dots of about one millimetre diameter, that were used in the targeting of the radiotherapy.
-
Missing Toenails - The nails on my big toes are missing, due to them being permanently removed to prevent an infection from reoccurring.
-
Hearing Difficulties - One of the chemotherapy drugs that I had during my second-line treatment, namely Cisplatin, damaged my hearing in a couple of ways. The damage consists of Tinnitus (a constant ringing sound) and loss of high frequencies; It is worse in my left ear. Whilst I don't notice it most of the time, as my idea of normal has gradually changed, I do struggle to pick-out voices in busier/noisier environments; Background noises, such as fans humming or numerous distant conversations, have a tendency to drowned-out nearby voices, especially women's voices.
-
Hair Loss - A number of the treatments have caused my hair to fall out, and whilst in the early days it eventually grew back, it is a lot thinner these days, hence being bald (or having really short hair) is about the only style that I can manage now, without giving away that something isn't quite right. Fortunately, I'm used to having short hair, so it doesn't bother me. In fact, I actually wish that it wouldn't grow at all, as it would be easier that way.
-
Scar Tissue - Despite the cancerous masses shrinking substantially as a result of the treatments I've had, there is still a significant amount of scar tissue left behind; It's similar to how if you inflate a balloon, and then let all of the air out, the balloon doesn't go back to its original size and shape. This doesn't pose a problem for myself, in that I can't tell that it's there, but it does complicate the interpretation of any medical imaging, as it can be hard to differentiate innocuous scar tissue from cancerous masses.
-
Weight Changes - The cancer and its treatment has caused my weight to drop overall, but not in a good way. Unfortunately, when your body is going through such a process, it is the lean muscle mass that it burns for its additional requirements. Also, even though you may be given steroids as part of your medications, which can dramatically increase your appetite, the type of steroids you're likely to be given (corticosteroids) don't help, as they often cause a redistribution of body fat to the face and torso, and with long-term use can lead to muscle wasting. (It's anabolic steroids that are used in bodybuilding, i.e. corticosteroids can have the opposite effect.)
-
Infertility - Most of the treatments affect fertility; For some it's likely to be a temporary side effect, but for others it's likely permanent. Whilst I've not actually been tested myself, it seems very unlikely that I will be fertile after all of the treatments that I've had. Fortunately, there are options such as adoption, should I ever want children, hence it is not a big issue for me.
-
Lung Damage - By comparing the results of my first and last lung function tests, you can see that my lungs have suffered from friendly-fire at times, as they don't work as well as they used to do. I'm only likely to notice the damage when my lungs have to work harder though, e.g. when exercising.
-
Peripheral Sensory Neuropathy - The monoclonal antibody-drug conjugate that I had during my third-line treatment, namely Brentuximab Vedotin, damaged the nerves in the extremities of my hands and feet. It's mostly my finger tips where I notice it now, as they often feel numb, tingly and tender. My fingers do tremble slightly at times now too, especially when performing tasks that require any precision or a light touch.
Finally wrapping this post up, hopefully the extensive albeit still incomplete description above gives you an appreciation for what I now consider to be my new normal; Hence, if you do ever bump in to me at the beach one day, and ask how I'm doing and say that I look well, you will know why I smile when replying: "I'm fine, thanks. How are you?"