It was probably about a year ago when I first noticed that there are variations between hospitals, as all of my prior treatment, right from the initial diagnosis in February 2009, had pretty much exclusively been at my local hospital in Cottingham; It was really only my PET-CT scans and hickman line insertions that had taken place at a different (also local) hospital in Hull, and that was purely down to those services not being available at the hospital in Cottingham. In other words, it was really only when I first visited a hospital in Leeds, and a month later started the process of switching my primary care to a hospital in Sheffield, that the variations between hospitals began to come to light.
The first difference that I noticed was that each of the hospitals had their own manual process for managing their clinics, i.e. keeping track of the patients etc, and that some were better than others when it came to things like informing the patients about their position in the queue. Given that I work in software development, it's likely of no great surprise that my thoughts turned to how these clinics could potentially benefit from some kind of computerised system, and I actually even created a quick demo of the kind of thing that I had in mind; I provided it to my local hospital in Cottingham as part of some feedback/suggestions that I sent them relating to my care over the years.
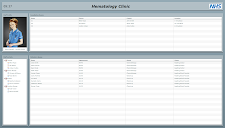
Note: There are a couple of screenshots of the demo below (click to view them full size), just in case you're curious what it looked like; The actual demo simulated the activity of a clinic, albeit sped-up, to give a better feel for how it would look/work. The idea was that what you can see in the screenshots would be on display in the waiting areas, so that everyone could see an overview of the clinic (screenshot on left) and patients could be alerted when a doctor was ready to see them (screenshot on right):
Making better use of modern technology has actually become somewhat of a recurring theme in the feedback/suggestions that I've provided to the hospitals responsible for my care, as it seems there are quite a number of processes/systems in hospitals that involve the use of paper and whiteboards etc, when a computerised approach would offer benefits such as easy archiving and backing-up, not to mention the potential to access that information from any device connected to the hospital's network.
The access to information, both electronic or otherwise, is another area that highlights the variations between hospitals, and how processes/systems are often more local than national, as it seems that, instead of centralised computer systems, numerous adhoc/individual solutions are quite common place; Hence, communication between hospitals in shared care situations can quickly become complicated, leading to things slipping through the cracks, and the quality of patient care rapidly deteriorating. You may recollect that the hospital in Sheffield were sometimes reluctant to share my care with my local hospital in Cottingham, due to concerns around miscommunication, and that a radiologist in Sheffield was unable to review one of my CT scans properly, due to not having access to the prior CT and PET-CT scans I'd had at other hospitals.
Taking a more centralised approach, thereby making the most of the health service's national status, would seem to be a beneficial change in other areas too, as even the purchasing of equipment and medication would appear to be managed more locally than nationally, based on discussions that I've had with some of the staff, and what I've seen used in the different hospitals. For example, even things like the connectors that are attached to my hickman line vary from one hospital to the next, when you'd likely expect the same ones to be used nationally, if only to secure a good deal on the price; I'm not sure whether there are any significant differences between them, but I put together the following image to show the four types (around the edge) that I've seen, as well as to show the cap (in the centre) that the hospital in Sheffield recently trialled; The latter aimed to reduce the number of infections introduced via central lines.
It's not just the brands/models of equipment that differs though, as occasionally what type is used does too. For example, with the exception of at my local hospital, my blood pressure has nearly always been measured using an automated machine, instead of manually with a stethoscope; My local hospital, after trialling the automated machines, came to the conclusion that the manual approach was better, as it was more accurate and gave the nurses control over how much pressure was applied to patients' arms, thereby enabling them to avoid bruising patients prone to such issues. Also, whilst my local hospital has always given me platelet transfusions without the use of an IV pump, apparently to avoid the platelets being crushed in the process, whenever I've had platelet transfusions in Sheffield an IV pump has always been used. In both instances, you'd likely expect a best practice to be agreed/used nationally.
Sometimes even the medication/treatment given varies between hospitals too. For example, the conditioning regimen that I would have been given for my Allogeneic Stem Cell Transplant (Allo-SCT) would have been different had I gone to the hospital in Leeds, instead of Sheffield. Whether one is any better than the other, in that particular instance at least, is probably not really known, due to insufficient evidence, but nevertheless you might expect to be treated the same throughout the NHS.
Note: Anthony Nolan, a charity that runs one of the UK's bone marrow registers, are currently trying to raise awareness of how post Allo-SCT care varies around the country, as can be seen in their associated news article and web page; One such variation being only some make use of ECP to treat GVHD. Incidentally, should you take a look at the report, the patient story on page thirty-four will likely sound familiar.
Putting aside the more clinical differences, it soon became apparent that the facilities being offered vary too. For example, TV, phone and/or Internet services aren't always available, and whilst in some places they are provided for free, in others the prices are extortionate. Also, whilst it's perhaps understandable that the price of parking ranges from free upwards, it seems odd that the factors that influence that, such as the type of treatment you are having, whether you have a disabled badge, and where you park, varies between hospitals. For both, you'd likely hope it was the same nationally.
Finally, there are a couple of other differences that stood-out too. The first, which in some ways probably surprised me the most, is that even the uniforms are different between hospitals. For example, in Sheffield the uniform worn by a qualified male nurse looks very similar to that worn at my local hospital by a student nurse - As you might imagine, that caused me some confusion initially, when nurses seemed to be doing jobs for which they weren't qualified. The second, which has at least on occasion provided a source of amusement, is that the catering differs too. For example, not only do the daily menus vary, but some hospitals out-source the catering whilst others do it themselves. If you are wondering what exactly is amusing about the catering, hopefully a couple of my recent orders will help to clear all of that up:
-
At my local hospital, when the breakfast trolley came around, I asked for Branflakes, only to find out that they had recently been removed from the menu. When I asked why, it turned-out that the reason was that patients often thought that Branflakes were the healthy option, when in reality they are sugar-coated. However, I could still order Frosties. I actually ordered some Cornflakes though, and proceeded to bury them in a tonne of sugar!
-
At the hospital in Sheffield, I recently ordered "Strawberry Jelly Rip" for my dessert, as that was the first time that I'd seen that on the menu, and I was curious what exactly would turn up. As you will no doubt appreciate from the photo below, there's a reason why it's not offered in chocolate flavour!