For the vast majority of patients diagnosed with Hodgkin's Lymphoma, the cancer is cured by the first-line treatment. However, for some patients, the cancer returns after the treatment (relapses) and/or proves to be resistant to the treatment (refractory). Fortunately, there are second-line and third-line treatments that can still potentially cure such patients, albeit with increasing toxicity and risks. Unfortunately, a few percent of patients ultimately fail all three lines of treatment. It's at that point where the goal of the treatment changes to controlling the cancer, rather than curing it. As you will know, if you've been following my blog, that's where I currently find myself, hence my timeline page shows a fairly typical treatment path for those unfortunate few.
When it came to choosing a treatment to control my cancer, the medical team at my local hospital considered three options: Vinblastine, Gemcitabine and Brentuximab Vedotin. Opinions were divided about which treatment was best, but Vinblastine was chosen in the end. Part of the reason why opinions were divided is that Hodgkin's Lymphoma is a relatively rare cancer to start with, hence when you consider that only a few percent of those diagnosed with it find themselves requiring such treatment, there are very few patients from which experience/knowledge can be gained, and consequently the evidence to show which treatment is best is somewhat lacking.
Note: Radiotherapy was ruled-out due to the Hodgkin's Lymphoma being in an area that has previously been irradiated, i.e. it would likely just cause more harm than good. Donor Lymphocyte Infusions (DLIs), which are a kind of boost of the donor's immune system, was also ruled-out due to the extent of the skin GVHD that I'd already acquired from the Allogeneic Stem Cell Transplant; If the donor's immune system was going to cure me, it would have done already, so DLIs would have just been asking for trouble.
It's perhaps not surprising that had my care been managed by another hospital, a different treatment might have been chosen. For example: the hospital that I attended on a few occasions in Leeds would have also considered the PECC regimen, but would have probably chosen Brentuximab Vedotin; and the hospital that I regularly attended in Sheffield would have also considered Bendamustine, but it's unclear what would have been chosen, as my local hospital had already opted for Vinblastine, and there were no strong feelings that something else would have been a better choice.
If you have been keeping track, you'll realise that's already five different treatments that might control Hodgkin's Lymphoma (albeit not indefinitely) in circumstances similar to my own. None of those treatments are currently considered to be potential cures, but in the case of Brentuximab Vedotin, it's not entirely clear whether that might change in the future. The reason being that Brentuximab Vedotin is quite a new treatment, hence more time is required for it to show its full potential; Having said that, there are patients for which it has been used to achieve ongoing remissions that are now approaching lengths where the medical community typically start to consider a patient as cured.
Over the last couple of years, it has become clear to myself from numerous online sources that there are several other treatments available too. The most commonly used seem to be: Everolimus (Afinitor), Lenalidomide (Revlimid), and Vorinostat (SAHA). Occasionally, even Rituximab (Rituxan) is used, as it appears to indirectly benefit some patients, presumably by targeting some of the cells around the cancer (microenvironment) that are helping to support it; In my case, that treatment might also help with the skin GVHD. More recently, Nivolumab has attracted a lot of interest, and a few months ago was actually granted the breakthrough therapy status by the FDA for Hodgkin's Lymphoma; It seems that Nivolumab and Ipilimumab work well as a combination too. In other words, there are quite a number of treatments available.
The existence of treatments that may help to control (if not cure) Hodgkin's Lymphoma is clearly a good thing, but, in some ways, the number of them can be problematic too, as it adds to the difficulty in deciding which to choose, especially when you consider that some of those treatments may have a synergistic effect when they're combined. For example, there are currently clinical trials taking place where the combination of Bendamustine and Brentuximab Vedotin is being investigated, as that may prove to be better than either of the drugs alone. There are many other clinical trials taking place too, often in the US, but until all of the evidence is in, it's a bit of a guessing game.
Whilst a number of the treatments that I've mentioned are of the more novel/targeted variety, i.e. not the typically more blunt/harsh instrument that is chemotherapy, that's not to say that they're without any risks or side effects. Consequently, whilst patients can (and do) jump from treatment to treatment, using each for as long as they prove beneficial, all of the time hoping for new breakthroughs/developments, our bodies are only capable of taking so much, hence eventually there is bound to be that straw that breaks the camel's back. The hope is simply that the cure comes before the straw!
A few years ago, a friend told me that I over-analyse things, but I'm not sure really; I'm still thinking about it.
Thursday 11 September 2014
Monday 1 September 2014
Sidelining cancer!
Given that a PET-CT scan had just confirmed that my Hodgkin's Lymphoma had relapsed, you might be asking yourself what spanner could I possibly throw in the works that would put cancer on the sideline. To answer that question I need to rewind time by a few months, back to the day that I tried to lift something out of a cupboard, only to find that it was jammed-in, and in the process hurt my back. At the time I never gave it much thought, as back injuries are nothing unusual, but with the wisdom of hindsight I can now see that it was perhaps the first sign of the problems to come.
Over the weeks that followed my back felt like it recovered a couple of times, but then I'd somehow manage to upset it again. Generally speaking, the pain wasn't too bad though, so the assumption was that it would get better with time. However, what did prove somewhat problematic was that I also had a cough; Likely due to the Influenza A that my immune system was struggling to eradicate. If you've ever had a back injury and a cough at the same time, you'll know that the two don't go well together.
For a while, I did my best to only cough when my back was supported, e.g. when sat in a chair, as the level of pain was much less that way. However, as much as I tried, sometimes I couldn't hold the cough in for long enough to ensure that the pain was minimal. There were a couple of particularly memorable occasions when I coughed and triggered an intense pain like nothing I've ever experienced before in my life; The pain would only start to subside when I took the weight off my back too, hence I quickly needed to somehow support myself with my arms before I collapsed in a heap.
One time, I grabbed hold of a door handle, all tensed-up and hardly able to breath, and froze there for what seemed like an eternity, until the pain eventually dropped enough that I could gradually start to relax and let go. The other time, I fell backwards on to my bed, yelled-out uncontrollably, rolled on to my side, and didn't dare move for about ten minutes. For the latter, I remember my back suddenly feeling hot, before the sensation faded and spread-out across my body, leaving most of me literally wet to the touch.
There had been an attempt to treat the Influenza A with Tamiflu, in the hope that it might ease the cough and allow my back to heal, but it didn't seem to help at all; If anything, it actually added to my symptoms. However, since having the Allogeneic Stem Cell Transplant, blood tests have shown that my lymphocytes have been fairly low, which is perhaps why I've picked-up a few viruses, hence the dose of my anti-viral medication was doubled; The lymphocytes in our immune system provide the main defence against viruses. It may have been coincidence, but after a few days of the increased dose of anti-viral medication I was coughing much less frequently.
Unfortunately, whilst not coughing as much certainly helped, the intense back pain could also be triggered by certain movements. For example, a couple of days before I got the PET-CT scan results, I was sat down, feeling fine, but then I bent-over to pick something up, and the pain I felt was excruciating. It was likely that incident that led to me being admitted into hospital a few days later, as afterwards trying to manage the pain using Oramorph alone simply wasn't working-out. The decision was made quite unexpectedly, because whilst I was on the phone with the hospital that day, it became clear to the nurse, just from my voice and the pauses in conversation, that sometimes I was struggling to speak, because the pain was quite literally taking my breath away.
On the day that I was admitted into hospital, I should have been starting my fifteenth ECP treatment, but it had been put on-hold whilst a treatment plan was determined for my Hodgkin's Lymphoma; I'd just started a five day course of high-dose steroids too, which meant that the ECP treatment was redundant in the short-term anyway, as we already knew that steroids were an effective way of treating my skin GVHD. Very little else actually happened that day, as I was pretty much pain free when sat in bed, and it was early evening when I got there, hence most of the doctors had gone home.
By the next day, the doctors at my local hospital had discussed potential treatments, and decided that Vinblastine chemotherapy was my best option. Given that I was now an inpatient, the plan was to start that treatment in the afternoon, whilst also adjusting my pain medication. However, the Vinblastine chemotherapy was delayed by a day, as I wanted to ask the doctors in Sheffield for their opinion, as they had managed my care for the last year and a half, hence it seemed sensible to see if they had any different ideas, given their expertise with Allogeneic Stem Cell Transplants etc. As it happened, they were happy to go with the Vinblastine chemotherapy, as it's difficult to say which of the potential treatments would be best, due to insufficient evidence. (I'll write more about the potential treatments, and the difficulties in choosing, in a separate post.)
Over the next few days or so, it was mostly a case of observing me to see how I got on, whilst tweaking my pain medication accordingly. It wasn't easy to decide how to proceed though, as there was no way to know whether any changes in my condition were a result of the high-dose steroids, chemotherapy, and/or pain medications. Also, given that I could be pain free one second, and in agony the next, it was difficult to know whether I was improving, without potentially causing myself quite a lot of pain. Fortunately, even though the days can feel long when you're just being observed, my local hospital provides a relaxing environment; This was the view from my room:
As you might imagine, the potential for severe spikes in pain meant that I was a bit weary of moving around. However, sometimes you don't really have any choice; For example, on one occasion, after going to toilet, I went to press the button to flush it and that triggered a horrendous pain. I quickly grabbed hold of some nearby handrails to hold myself up with my arms, thereby relieving some of the pain, but I couldn't let go without it returning. Clearly, I couldn't stay there either; I had to somehow call for help.
Of course, the problem was how to call for help, as even if I was able to shout, I doubt anyone would have heard me, so that only left setting the buzzer off to call for a nurse. There happened to be a button to do that next to the toilet, hence it looked like my best option. It took me about five minutes, and far more pain than I would have liked, to get sat down on the toilet, where I was finally able to reach the button, and even then I still had to support myself with my arms, hence I struggled to actually press it. Fortunately, it wasn't long before a nurse arrived, and I could take some additional pain relief; Once it had kicked-in, I made my way back to my bed, with the help of a zimmer frame.
After that experience, I wasn't going to try walking anywhere without first calling for a nurse, just in case I needed help. However, even that didn't work out very well, as the first time that I tried it, I only managed a couple of steps before the pain kicked-in, I yelled-out uncontrollably, and both the nurse and myself found ourselves stuck. I was holding myself up with the help of a cupboard on my right, and the nurse on my left. Consequently, the nurse was unable to call for help, much like I had been previously. Without really thinking, I just stumbled backwards towards the bed and sat down, albeit not very elegantly. The nurse then shot-off to get some pain relief and colleagues to help. I think I scared the poor nurse to death; Even though I had tried to explain what might happen, I don't think I'd quite managed to describe the extent of the problem.
Given the ongoing issues that I was having with the back pain, despite the steroids, chemotherapy and pain relief, the doctors decided that I needed an MRI scan of my spine to see whether that highlighted any potential causes. I wasn't exactly thrilled with the idea, as my last PET-CT scan had been quite an unpleasant experience, due to the back pain, and I'd only got worse since then. However, there wasn't really an alternative, and it did mean that I would finally find out what an MRI scan is like. (I'll write about MRI scanners, and my experience of being in one, in a separate post.)
By the time I had the MRI scan, I'd been in hospital for a week, and during that time there had been a couple of theories about the cause of my back pain: The Hodgkin's Lymphoma could have spread to my spine, or the steroids I'd been taking might have weakened my bones, thereby making it easy to damage them. After much debate, and specialists getting involved, the results of my recent scans led to the conclusion that I had compression fractures on seven vertebrae in my lower back (T11-T12 and L1-L5).
Note: The CT scan didn't show anything of interest, the PET-CT scan showed some activity on one of my vertebrae (T11), and the MRI scan showed that seven vertebrae were crumbling at the top and bottom. Although CT and PET-CT scans are not very good for identifying these kind of issues, it appeared that as time was progressing, I'd been causing more damage. Therefore, the plan was to have a procedure known as a multi-level Vertobroplasty, in order to strengthen the damaged vertebrae and in doing so relieve the pain. (I'll write about the multi-level Vertobroplasty in a separate post.)
For various reasons, it was just over two weeks after the MRI scan before I actually went for the multi-level Vertobroplasty, during which time I was pretty much stuck in my hospital bed, as it wasn't safe for me to walk around. I did occasionally slide on to a wheelchair, so that I could go to the bathroom to get washed etc. A physiotherapist also came to see me on most days, so that I could try to walk a few steps with the help of a zimmer frame. However, sometimes I wasn't well enough, either because I'd upset my back from getting washed etc, or because the day after the MRI scan I'd picked-up an infection, and needed IV antibiotics for a week to help to clear it up.
Note: The sudden change in my mobility made me realise how much I'd always taken the ability to perform even the simplest of tasks for granted, e.g. picking-up things that I'd dropped on the floor or reaching for things on high shelves, hence being dependent on others for such tasks was definitely an adjustment. I know that I soon acquired a newfound respect for those that are unable to walk; It's quite surprising in how many ways all sorts of things are not designed with that thought in mind. For example, I even struggled to get out of a hospital bathroom one day, as the door was pretty heavy/stiff, and that made it difficult to push open when sat in a wheelchair (with a bad back).
Fortunately, the multi-level Vertebroplasty made a huge difference to the back pain, but as you might imagine the procedure itself required some recovery time, which meant that it wasn't until five days later (making it a four week long stay) that I was finally able to go home. Having said that, it was my circumstances that influenced the recovery time, as after spending so many days in a hospital bed, I'd lost a lot of my strength; My legs were so weak that I could barely walk. Also, the chemotherapy that I was having was causing me to be anemic, which meant that I was easily out-of-breath, hence anything remotely physical was just that bit harder. (As it happened, my second dose of the chemotherapy was a couple of days after the multi-level Vertebroplasty.)
In the couple of months that followed, the Vinblastine chemotherapy every two weeks (as an outpatient) was essentially my only treatment; I had my sixth dose just a few days ago. The Vinblastine chemotherapy has occasionally meant that I've needed blood transfusions, due to being anemic, and regular injections of Filgrastim (G-CSF) to boost my immune system, due to being neutropenic, but beyond that it has proven to be a fairly easy-going treatment. Having said that: I did pick-up an infection in late July, which meant spending a few days as an inpatient on IV antibiotics followed by a course of oral antibiotics at home; my hair has thinned even more; my peripheral sensory neuropathy (mostly numb/tingly/tender finger tips) has got a bit worse; and I've needed to add Movicol and Senna to my mini pharmacy due to constipation.
Note: Initially, in addition to the Vinblastine chemotherapy, the treatment plan also included periodic short courses of high-dose steroids. However, given that I was already taking steroids to help with controlling my skin GVHD, the decision was made to just increase my regular dose to 20mg/day instead; Prior to starting ECP, that dose proved to be just enough. (I did actually taper-down to my 10mg/day dose for a few days, with a couple of days at 25mg/day, before that decision was made though.)
Unfortunately, even though I've tolerated the Vinblastine chemotherapy fairly well, I've still struggled with my mobility, due to the need to regain my strength and ongoing issues with either back or hip pain, post the multi-level Vertebroplasty. It seems like the pain has been in different places to those strengthened though, once I'd had a bit of time to recover, and in the vast majority of cases hasn't been as bad. However, it has been somewhat of a bumpy road, and perhaps surprisingly continues to be more problematic than the cancer! (I even have various mobility aids in my house now!)
Over the weeks that followed my back felt like it recovered a couple of times, but then I'd somehow manage to upset it again. Generally speaking, the pain wasn't too bad though, so the assumption was that it would get better with time. However, what did prove somewhat problematic was that I also had a cough; Likely due to the Influenza A that my immune system was struggling to eradicate. If you've ever had a back injury and a cough at the same time, you'll know that the two don't go well together.
For a while, I did my best to only cough when my back was supported, e.g. when sat in a chair, as the level of pain was much less that way. However, as much as I tried, sometimes I couldn't hold the cough in for long enough to ensure that the pain was minimal. There were a couple of particularly memorable occasions when I coughed and triggered an intense pain like nothing I've ever experienced before in my life; The pain would only start to subside when I took the weight off my back too, hence I quickly needed to somehow support myself with my arms before I collapsed in a heap.
One time, I grabbed hold of a door handle, all tensed-up and hardly able to breath, and froze there for what seemed like an eternity, until the pain eventually dropped enough that I could gradually start to relax and let go. The other time, I fell backwards on to my bed, yelled-out uncontrollably, rolled on to my side, and didn't dare move for about ten minutes. For the latter, I remember my back suddenly feeling hot, before the sensation faded and spread-out across my body, leaving most of me literally wet to the touch.
There had been an attempt to treat the Influenza A with Tamiflu, in the hope that it might ease the cough and allow my back to heal, but it didn't seem to help at all; If anything, it actually added to my symptoms. However, since having the Allogeneic Stem Cell Transplant, blood tests have shown that my lymphocytes have been fairly low, which is perhaps why I've picked-up a few viruses, hence the dose of my anti-viral medication was doubled; The lymphocytes in our immune system provide the main defence against viruses. It may have been coincidence, but after a few days of the increased dose of anti-viral medication I was coughing much less frequently.
Unfortunately, whilst not coughing as much certainly helped, the intense back pain could also be triggered by certain movements. For example, a couple of days before I got the PET-CT scan results, I was sat down, feeling fine, but then I bent-over to pick something up, and the pain I felt was excruciating. It was likely that incident that led to me being admitted into hospital a few days later, as afterwards trying to manage the pain using Oramorph alone simply wasn't working-out. The decision was made quite unexpectedly, because whilst I was on the phone with the hospital that day, it became clear to the nurse, just from my voice and the pauses in conversation, that sometimes I was struggling to speak, because the pain was quite literally taking my breath away.
On the day that I was admitted into hospital, I should have been starting my fifteenth ECP treatment, but it had been put on-hold whilst a treatment plan was determined for my Hodgkin's Lymphoma; I'd just started a five day course of high-dose steroids too, which meant that the ECP treatment was redundant in the short-term anyway, as we already knew that steroids were an effective way of treating my skin GVHD. Very little else actually happened that day, as I was pretty much pain free when sat in bed, and it was early evening when I got there, hence most of the doctors had gone home.
By the next day, the doctors at my local hospital had discussed potential treatments, and decided that Vinblastine chemotherapy was my best option. Given that I was now an inpatient, the plan was to start that treatment in the afternoon, whilst also adjusting my pain medication. However, the Vinblastine chemotherapy was delayed by a day, as I wanted to ask the doctors in Sheffield for their opinion, as they had managed my care for the last year and a half, hence it seemed sensible to see if they had any different ideas, given their expertise with Allogeneic Stem Cell Transplants etc. As it happened, they were happy to go with the Vinblastine chemotherapy, as it's difficult to say which of the potential treatments would be best, due to insufficient evidence. (I'll write more about the potential treatments, and the difficulties in choosing, in a separate post.)
Over the next few days or so, it was mostly a case of observing me to see how I got on, whilst tweaking my pain medication accordingly. It wasn't easy to decide how to proceed though, as there was no way to know whether any changes in my condition were a result of the high-dose steroids, chemotherapy, and/or pain medications. Also, given that I could be pain free one second, and in agony the next, it was difficult to know whether I was improving, without potentially causing myself quite a lot of pain. Fortunately, even though the days can feel long when you're just being observed, my local hospital provides a relaxing environment; This was the view from my room:
As you might imagine, the potential for severe spikes in pain meant that I was a bit weary of moving around. However, sometimes you don't really have any choice; For example, on one occasion, after going to toilet, I went to press the button to flush it and that triggered a horrendous pain. I quickly grabbed hold of some nearby handrails to hold myself up with my arms, thereby relieving some of the pain, but I couldn't let go without it returning. Clearly, I couldn't stay there either; I had to somehow call for help.
Of course, the problem was how to call for help, as even if I was able to shout, I doubt anyone would have heard me, so that only left setting the buzzer off to call for a nurse. There happened to be a button to do that next to the toilet, hence it looked like my best option. It took me about five minutes, and far more pain than I would have liked, to get sat down on the toilet, where I was finally able to reach the button, and even then I still had to support myself with my arms, hence I struggled to actually press it. Fortunately, it wasn't long before a nurse arrived, and I could take some additional pain relief; Once it had kicked-in, I made my way back to my bed, with the help of a zimmer frame.
After that experience, I wasn't going to try walking anywhere without first calling for a nurse, just in case I needed help. However, even that didn't work out very well, as the first time that I tried it, I only managed a couple of steps before the pain kicked-in, I yelled-out uncontrollably, and both the nurse and myself found ourselves stuck. I was holding myself up with the help of a cupboard on my right, and the nurse on my left. Consequently, the nurse was unable to call for help, much like I had been previously. Without really thinking, I just stumbled backwards towards the bed and sat down, albeit not very elegantly. The nurse then shot-off to get some pain relief and colleagues to help. I think I scared the poor nurse to death; Even though I had tried to explain what might happen, I don't think I'd quite managed to describe the extent of the problem.
Given the ongoing issues that I was having with the back pain, despite the steroids, chemotherapy and pain relief, the doctors decided that I needed an MRI scan of my spine to see whether that highlighted any potential causes. I wasn't exactly thrilled with the idea, as my last PET-CT scan had been quite an unpleasant experience, due to the back pain, and I'd only got worse since then. However, there wasn't really an alternative, and it did mean that I would finally find out what an MRI scan is like. (I'll write about MRI scanners, and my experience of being in one, in a separate post.)
By the time I had the MRI scan, I'd been in hospital for a week, and during that time there had been a couple of theories about the cause of my back pain: The Hodgkin's Lymphoma could have spread to my spine, or the steroids I'd been taking might have weakened my bones, thereby making it easy to damage them. After much debate, and specialists getting involved, the results of my recent scans led to the conclusion that I had compression fractures on seven vertebrae in my lower back (T11-T12 and L1-L5).
Note: The CT scan didn't show anything of interest, the PET-CT scan showed some activity on one of my vertebrae (T11), and the MRI scan showed that seven vertebrae were crumbling at the top and bottom. Although CT and PET-CT scans are not very good for identifying these kind of issues, it appeared that as time was progressing, I'd been causing more damage. Therefore, the plan was to have a procedure known as a multi-level Vertobroplasty, in order to strengthen the damaged vertebrae and in doing so relieve the pain. (I'll write about the multi-level Vertobroplasty in a separate post.)
For various reasons, it was just over two weeks after the MRI scan before I actually went for the multi-level Vertobroplasty, during which time I was pretty much stuck in my hospital bed, as it wasn't safe for me to walk around. I did occasionally slide on to a wheelchair, so that I could go to the bathroom to get washed etc. A physiotherapist also came to see me on most days, so that I could try to walk a few steps with the help of a zimmer frame. However, sometimes I wasn't well enough, either because I'd upset my back from getting washed etc, or because the day after the MRI scan I'd picked-up an infection, and needed IV antibiotics for a week to help to clear it up.
Note: The sudden change in my mobility made me realise how much I'd always taken the ability to perform even the simplest of tasks for granted, e.g. picking-up things that I'd dropped on the floor or reaching for things on high shelves, hence being dependent on others for such tasks was definitely an adjustment. I know that I soon acquired a newfound respect for those that are unable to walk; It's quite surprising in how many ways all sorts of things are not designed with that thought in mind. For example, I even struggled to get out of a hospital bathroom one day, as the door was pretty heavy/stiff, and that made it difficult to push open when sat in a wheelchair (with a bad back).
Fortunately, the multi-level Vertebroplasty made a huge difference to the back pain, but as you might imagine the procedure itself required some recovery time, which meant that it wasn't until five days later (making it a four week long stay) that I was finally able to go home. Having said that, it was my circumstances that influenced the recovery time, as after spending so many days in a hospital bed, I'd lost a lot of my strength; My legs were so weak that I could barely walk. Also, the chemotherapy that I was having was causing me to be anemic, which meant that I was easily out-of-breath, hence anything remotely physical was just that bit harder. (As it happened, my second dose of the chemotherapy was a couple of days after the multi-level Vertebroplasty.)
In the couple of months that followed, the Vinblastine chemotherapy every two weeks (as an outpatient) was essentially my only treatment; I had my sixth dose just a few days ago. The Vinblastine chemotherapy has occasionally meant that I've needed blood transfusions, due to being anemic, and regular injections of Filgrastim (G-CSF) to boost my immune system, due to being neutropenic, but beyond that it has proven to be a fairly easy-going treatment. Having said that: I did pick-up an infection in late July, which meant spending a few days as an inpatient on IV antibiotics followed by a course of oral antibiotics at home; my hair has thinned even more; my peripheral sensory neuropathy (mostly numb/tingly/tender finger tips) has got a bit worse; and I've needed to add Movicol and Senna to my mini pharmacy due to constipation.
Note: Initially, in addition to the Vinblastine chemotherapy, the treatment plan also included periodic short courses of high-dose steroids. However, given that I was already taking steroids to help with controlling my skin GVHD, the decision was made to just increase my regular dose to 20mg/day instead; Prior to starting ECP, that dose proved to be just enough. (I did actually taper-down to my 10mg/day dose for a few days, with a couple of days at 25mg/day, before that decision was made though.)
Unfortunately, even though I've tolerated the Vinblastine chemotherapy fairly well, I've still struggled with my mobility, due to the need to regain my strength and ongoing issues with either back or hip pain, post the multi-level Vertebroplasty. It seems like the pain has been in different places to those strengthened though, once I'd had a bit of time to recover, and in the vast majority of cases hasn't been as bad. However, it has been somewhat of a bumpy road, and perhaps surprisingly continues to be more problematic than the cancer! (I even have various mobility aids in my house now!)
Wednesday 13 August 2014
Hodgkin's Lymphoma - Take Four!
A couple of days after my previous post, I woke-up in the middle of the night with pain in the right side of my chest. It was actually the second time that I'd done so; The first time was a few days previous. On the first occasion, it took me about half an hour to simply get sat-up, so that I could reach the phone to check with the hospital what I needed to do; It took that long as the pain in my chest increased substantially upon certain movements. Part of what made sitting-up especially difficult was that in the weeks prior to that I'd also been suffering from lower back pain, hence trying to find a way to sit-up without hurting either my back or my chest proved to be a challenge.
When I spoke to the hospital about the pain that I was experiencing, they suspected that it was likely just muscular pain, and that some painkillers should help to take the edge off the pain whilst I recovered naturally. However, with the chest pain occurring again, a few days later, and that it happened to coincide with an appointment for some routine blood tests etc, I asked to see one of the doctors whilst I was there, so that I could get checked over in person; i.e. not rely on my description over the phone.
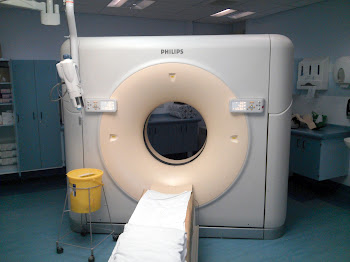
As it happened, I'd had a routine CT scan a week previous, just to check that everything still looked fine, which I was yet to hear the results from, hence I asked whether the CT scan showed any potential causes of the pain. Unfortunately, at that point, the doctor was unable to view the CT scan, and a radiologist was yet to write the associated report to go along with it, hence I needed to have an x-ray. Once I got back from the x-ray, the doctor had somehow managed to view the CT scan, and could see that there was something in the right side of my chest; Possibly a pleural effusion (fluid around a lung). That meant I needed to be admitted, so that the fluid could be drained the next day, once the doctor had discussed the CT scan with a colleague/radiologist. Incidentally, if you've never seen a CT scanner, I recently took this photo of one:
The next day, I was actually just discharged, as after further discussion had taken place, it was decided that I needed to have a PET-CT scan, and the next available slot for doing so would probably be in about a week. The rationale for the PET-CT scan was that what the CT scan showed wasn't entirely consistent with a pleural effusion, as the fluid wasn't quite everywhere that would be expected should that have been the case, hence it was looking more like yet another relapse of my Hodgkin's Lymphoma; i.e. the PET-CT scan would provide the additional information necessary to decide.
Note: In terms of the chest pain, I'd noticed that the days when it occurred seemed to coincide with the days when I was due a lower dose of steroids, hence I asked about amending my steroid dosage. The doctor was happy for me to try changing my steroid dose to 10mg/day, rather than a three day cycle of 5mg, 10mg and 10mg, as it was only a minor change, so it was unlikely to affect the results of the PET-CT scan. The change did prove to be enough to resolve the issue with the chest pain though.
Fortunately, spending the night in my local hospital, even if it does turn-out to be unnecessary, doesn't bother me, as the staff, ward and setting are all nice; In fact, given how much time I've spent there in recent years, it's almost like my second home. Plus, in the early evening, if you take a look out of your window, all that you're missing from watching a wildlife documentary is David Attenborough narrating; I did get a photo of one such visitor, when it came fairly close (click to view it full size):
It was just under a week later when I had the PET-CT scan, which turned-out to be not the nicest of experiences, as whilst laying down on the scanner only caused fairly mild back pain, and the PET-CT scan itself was fine, actually getting off the scanner was an entirely different story. Fortunately, the technician was especially helpful, not to mention patient, and between us we managed to find a way to get me off the scanner without it being too traumatic; It took about a quarter of an hour though, and there were a few sudden, sharp spikes in pain that definitely stopped me dead in my tracks.
When I got the results of the PET-CT scan, just under a week later, it was clear that my Hodgkin's Lymphoma had relapsed. Consequently, the doctor explained that because I've already had all of the treatments that are currently considered to be potential cures, all that was really left now was trying to control the cancer for as long as possible, using treatments that tend to be well-tolerated; i.e. allow for a good quality of life. No-one can really say how long or short that life will be; It could be several weeks, months or years. However, what the doctor did say was that eventually the Hodgkin's Lymphoma is going to kill me. Obviously, the doctor doesn't know that with absolute certainty, as a new treatment could be developed that does cure me, or I could get run-over by a bus, but clearly the prognosis was far from being good.
Note: Over the previous few months, there had been several signs that my Hodgkin's Lymphoma had relapsed, hence confirmation of that wasn't an entirely unexpected result of the scans. The problem is that often there are several potential explanations for a symptom. Some examples being: I had been itching, but that could have been from the skin GVHD; I had been coughing, but that could have been from the Influenza A that my immune system was struggling to eradicate; and blood tests showed that my erythrocyte sedimentation rate (ESR) was elevated, but it's just a non-specific measure of inflammation, hence that could have been from my big toes healing after the nails were permanently removed. Having said that, blood tests also showed that my lactate dehydrogenase (LDH) was gradually increasing; An elevated LDH is a potential indicator of Hodgkin's Lymphoma, hence it made me the most suspicious.
To give myself time to digest the news, as well as the various medical professionals involved in my case the opportunity to debate what is best to do next, we only briefly discussed what my treatment plan might look like going forwards, before arranging another appointment, for a few days later, where we would both be in a better position to go over the details. We did also organise some pain relief for my lower back, which would be reviewed at my next appointment, and agreed to increase my steroid dose to 100mg/day for five days, as that should help with treating the Hodgkin's Lymphoma.
Note: The pain relief was in the form of morphine sulphate solution (Oramorph); It quickly (20-30 minutes) relieves severe pain for a short period (3-6 hours). The idea being that it can be taken as/when required (within reason), as a way to determine the dose needed on a typical day. That Oramorph dose can then be replaced with the equivalent dose of morphine sulphate tablets (MST); MST is easier to administrate and acts over a longer period (8-12 hours), giving a more consistent level of pain relief. At which point, the Oramorph need only be used to cover any increases in pain.
Whilst the appointment in a few days' time seemed like a perfectly reasonable plan, it was only the next day that I threw a spanner in the works, and consequently was admitted to my local hospital. I was an inpatient for much longer than I expected, but that's a story for another post, as this one is long enough already. In the mean time, you can get a sneak preview by taking a look at the timeline page that I recently added to my blog - It lists my treatment history, from the very beginning to the present day.
When I spoke to the hospital about the pain that I was experiencing, they suspected that it was likely just muscular pain, and that some painkillers should help to take the edge off the pain whilst I recovered naturally. However, with the chest pain occurring again, a few days later, and that it happened to coincide with an appointment for some routine blood tests etc, I asked to see one of the doctors whilst I was there, so that I could get checked over in person; i.e. not rely on my description over the phone.
As it happened, I'd had a routine CT scan a week previous, just to check that everything still looked fine, which I was yet to hear the results from, hence I asked whether the CT scan showed any potential causes of the pain. Unfortunately, at that point, the doctor was unable to view the CT scan, and a radiologist was yet to write the associated report to go along with it, hence I needed to have an x-ray. Once I got back from the x-ray, the doctor had somehow managed to view the CT scan, and could see that there was something in the right side of my chest; Possibly a pleural effusion (fluid around a lung). That meant I needed to be admitted, so that the fluid could be drained the next day, once the doctor had discussed the CT scan with a colleague/radiologist. Incidentally, if you've never seen a CT scanner, I recently took this photo of one:
The next day, I was actually just discharged, as after further discussion had taken place, it was decided that I needed to have a PET-CT scan, and the next available slot for doing so would probably be in about a week. The rationale for the PET-CT scan was that what the CT scan showed wasn't entirely consistent with a pleural effusion, as the fluid wasn't quite everywhere that would be expected should that have been the case, hence it was looking more like yet another relapse of my Hodgkin's Lymphoma; i.e. the PET-CT scan would provide the additional information necessary to decide.
Note: In terms of the chest pain, I'd noticed that the days when it occurred seemed to coincide with the days when I was due a lower dose of steroids, hence I asked about amending my steroid dosage. The doctor was happy for me to try changing my steroid dose to 10mg/day, rather than a three day cycle of 5mg, 10mg and 10mg, as it was only a minor change, so it was unlikely to affect the results of the PET-CT scan. The change did prove to be enough to resolve the issue with the chest pain though.
Fortunately, spending the night in my local hospital, even if it does turn-out to be unnecessary, doesn't bother me, as the staff, ward and setting are all nice; In fact, given how much time I've spent there in recent years, it's almost like my second home. Plus, in the early evening, if you take a look out of your window, all that you're missing from watching a wildlife documentary is David Attenborough narrating; I did get a photo of one such visitor, when it came fairly close (click to view it full size):
It was just under a week later when I had the PET-CT scan, which turned-out to be not the nicest of experiences, as whilst laying down on the scanner only caused fairly mild back pain, and the PET-CT scan itself was fine, actually getting off the scanner was an entirely different story. Fortunately, the technician was especially helpful, not to mention patient, and between us we managed to find a way to get me off the scanner without it being too traumatic; It took about a quarter of an hour though, and there were a few sudden, sharp spikes in pain that definitely stopped me dead in my tracks.
When I got the results of the PET-CT scan, just under a week later, it was clear that my Hodgkin's Lymphoma had relapsed. Consequently, the doctor explained that because I've already had all of the treatments that are currently considered to be potential cures, all that was really left now was trying to control the cancer for as long as possible, using treatments that tend to be well-tolerated; i.e. allow for a good quality of life. No-one can really say how long or short that life will be; It could be several weeks, months or years. However, what the doctor did say was that eventually the Hodgkin's Lymphoma is going to kill me. Obviously, the doctor doesn't know that with absolute certainty, as a new treatment could be developed that does cure me, or I could get run-over by a bus, but clearly the prognosis was far from being good.
Note: Over the previous few months, there had been several signs that my Hodgkin's Lymphoma had relapsed, hence confirmation of that wasn't an entirely unexpected result of the scans. The problem is that often there are several potential explanations for a symptom. Some examples being: I had been itching, but that could have been from the skin GVHD; I had been coughing, but that could have been from the Influenza A that my immune system was struggling to eradicate; and blood tests showed that my erythrocyte sedimentation rate (ESR) was elevated, but it's just a non-specific measure of inflammation, hence that could have been from my big toes healing after the nails were permanently removed. Having said that, blood tests also showed that my lactate dehydrogenase (LDH) was gradually increasing; An elevated LDH is a potential indicator of Hodgkin's Lymphoma, hence it made me the most suspicious.
To give myself time to digest the news, as well as the various medical professionals involved in my case the opportunity to debate what is best to do next, we only briefly discussed what my treatment plan might look like going forwards, before arranging another appointment, for a few days later, where we would both be in a better position to go over the details. We did also organise some pain relief for my lower back, which would be reviewed at my next appointment, and agreed to increase my steroid dose to 100mg/day for five days, as that should help with treating the Hodgkin's Lymphoma.
Note: The pain relief was in the form of morphine sulphate solution (Oramorph); It quickly (20-30 minutes) relieves severe pain for a short period (3-6 hours). The idea being that it can be taken as/when required (within reason), as a way to determine the dose needed on a typical day. That Oramorph dose can then be replaced with the equivalent dose of morphine sulphate tablets (MST); MST is easier to administrate and acts over a longer period (8-12 hours), giving a more consistent level of pain relief. At which point, the Oramorph need only be used to cover any increases in pain.
Whilst the appointment in a few days' time seemed like a perfectly reasonable plan, it was only the next day that I threw a spanner in the works, and consequently was admitted to my local hospital. I was an inpatient for much longer than I expected, but that's a story for another post, as this one is long enough already. In the mean time, you can get a sneak preview by taking a look at the timeline page that I recently added to my blog - It lists my treatment history, from the very beginning to the present day.
Sunday 25 May 2014
How can I help save someone's life?
As you may know, on the 31st of January 2013, a complete stranger's stem cells were being dripped into my bloodstream. The hope being that once they had taken over the production of my blood, I might have an immune system that was capable of curing my Hodgkin's Lymphoma. A few months later, that hope was shown to be the reality by a PET-CT scan, and, just over a year further down the line, that is still the case. It hasn't been the smoothest of journeys, but I'm here to tell the tale, and in all likelihood that's only because an act of kindness from a complete stranger saved my life!
You could be the complete stranger saving someone else's life one day, if you're in good health and aged between 16 and 49 (inclusive). In the vast majority of cases, doing so is almost as simple as donating blood. You can read about what is involved in one of my earlier blog posts: How can I donate stem cells or bone marrow?
Whether you can be a donor or not, maybe you could save yourself some money, whilst at the same time helping to raise funds for the Anthony Nolan charity, which operates one of the registers for donors in the UK. You might be thinking that sounds too good to be true, but surprisingly it's not, as a couple of the services that I use, for which you could sign-up, operate a referral scheme, and any proceeds that I earn from those referral schemes I'll donate to the Anthony Nolan charity. It's that simple!
You can also take a look at the Anthony Nolan website for other ways to help. Perhaps you'd like to get involved with fundraising, or even just donate money yourself? Maybe you'd like to be one of Anthony Nolan's volunteers? If you're pregnant, you could even consider donating the blood from your umbilical cord and placenta! More information about all of those possibilities (and more) is available on the Anthony Nolan website.
You could be the complete stranger saving someone else's life one day, if you're in good health and aged between 16 and 49 (inclusive). In the vast majority of cases, doing so is almost as simple as donating blood. You can read about what is involved in one of my earlier blog posts: How can I donate stem cells or bone marrow?
Whether you can be a donor or not, maybe you could save yourself some money, whilst at the same time helping to raise funds for the Anthony Nolan charity, which operates one of the registers for donors in the UK. You might be thinking that sounds too good to be true, but surprisingly it's not, as a couple of the services that I use, for which you could sign-up, operate a referral scheme, and any proceeds that I earn from those referral schemes I'll donate to the Anthony Nolan charity. It's that simple!
- TopCashback is a free service that essentially offers savings on a wide range of online purchases, and it couldn't be any easier to use; The few extra seconds that it takes you can sometimes offer substantial savings. Just today, I saved £22.22 on my home insurance, and earned £5.59 for simply getting quotes from three different home insurance comparison websites! In the last four and a half years, I've saved/earned nearly £700! Currently, if you sign-up via My TopCashback Referral Page, you will get a £5 Marks & Spencer's eGift card, and I'll get £10 to donate on your behalf, once you have saved/earned £10 via their free service.
- GiffGaff is a mobile phone service provider, powered by O2, with prices that tend to compare very favourably to that of the various others available. Their service is operated slightly differently, the result of which tends to provide extra flexibility for yourself, even though you do essentially still choose between pay as you go or a monthly contract. Currently, if you sign-up via My GiffGaff Referral Page, you will get £5 credit, and I'll get £5 to donate on your behalf, once you have added £10 to your credit.
You can also take a look at the Anthony Nolan website for other ways to help. Perhaps you'd like to get involved with fundraising, or even just donate money yourself? Maybe you'd like to be one of Anthony Nolan's volunteers? If you're pregnant, you could even consider donating the blood from your umbilical cord and placenta! More information about all of those possibilities (and more) is available on the Anthony Nolan website.
Monday 28 April 2014
What was having your big toenails removed like?
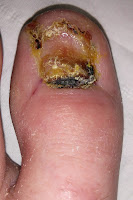
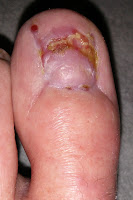
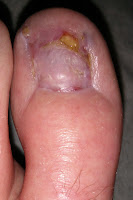
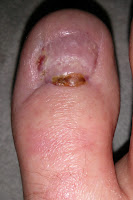
In an earlier post, I promised to share some photos of what my big toes looked like after the nails had been permanently removed by an orthopedic surgeon. You might wish that I'd forgotten about my promise, especially after you see the photos, but I'm fulfilling it anyway! In fact, I've actually gone a step further, as for about the last four months I've taken a photo of them every couple of weeks, hence not only can you see how they looked initially, you can also see exactly how they've been healing!
Note: Prior to having my big toenails removed, I was told that the healing process takes between six and twelve weeks for your typical patient, but that it would in all likelihood take a little longer for myself, due to my medical history; As you no doubt remember, I currently take steroids to help keep my skin GVHD under control, and, unfortunately, not only do they increase my risk of infection, they also impair my ability to heal. In other words, the steroids make the procedure riskier and recovery longer!
In the early stages of the recovery, one of the nurses commented that my big toes were taking their time to dry-out/scab-over, which meant that I needed to use some iodine dressings for a number of weeks to speed-up that process. I was expecting the iodine dressings to sting quite a bit, but they didn't actually feel any different to the normal dressings really. Having said that, neither were particularly comfortable!
In an earlier post, there was a photo of the extensive dressings used initially, and another of the radically scaled-down dressings used after a week or so, and below there is a photo of the plasters (with some gauze underneath for padding etc) that I've used for approximately the last two months. If you view the photo below full size, by simply clicking on it, you will also see how the skin GVHD is affecting my feet, despite the creams, medications and Extracorporeal Photopheresis (ECP) used to treat it.
The various dressings used over the last four months have all needed to be kept dry, which has meant that I've only been able to get a shower when the dressings were due to be changed. Initially that was once per week, and later on twice per week, as changing the dressings too frequently (particularly in the early stages) impairs the healing process. As you might imagine, getting washed with a flannel on the other days has certainly given me a newfound appreciation for the inventor of showers!
Whilst the dressings do help to mask the sensitivity of the wounds, even wearing socks can still be slightly uncomfortable, as the stitching tends to be exactly where the wound is most sensitive. Having said that, what really made my big toes throb was if I didn't keep my feet elevated. It seemed like standing-up and walking around etc would make my big toes swell, and that resulted in the dressings applying more pressure.
It has only been in the last month or so that I've started to wear my trainers again, instead of the blue strap-on boots (see the photo below) provided by the hospital, as even though my big toes didn't look too bad after a couple of months, they were still quite sensitive, hence avoiding any pressure on them was far more comfortable. In fact, even now my big toes are still a little bit sensitive, but that should gradually fade over time as the skin hardens. Interestingly, once the skin has hardened, my big toes should be just as well-protected as when they had nails; Toenails don't really serve any purpose these days, so the only consequence of their removal is you have less to cut!
Fortunately, my big toes mostly feel fine now, albeit still slightly sensitive. As you no doubt noticed from the photos above, even after eighteen weeks, my big toes still have a small amount of healing left to do (more so on my right foot than my left foot), but I'm now really just hoping that the orthopedic surgeon managed to completely remove all traces of my big toenails, as I really don't want part of them to start growing back again. I'd like to be able to draw a line under the whole ingrowing toenails saga!
Note: Prior to having my big toenails removed, I was told that the healing process takes between six and twelve weeks for your typical patient, but that it would in all likelihood take a little longer for myself, due to my medical history; As you no doubt remember, I currently take steroids to help keep my skin GVHD under control, and, unfortunately, not only do they increase my risk of infection, they also impair my ability to heal. In other words, the steroids make the procedure riskier and recovery longer!
Big Toenail Removal - Left Foot
Big Toenail Removal - Right Foot
In an earlier post, there was a photo of the extensive dressings used initially, and another of the radically scaled-down dressings used after a week or so, and below there is a photo of the plasters (with some gauze underneath for padding etc) that I've used for approximately the last two months. If you view the photo below full size, by simply clicking on it, you will also see how the skin GVHD is affecting my feet, despite the creams, medications and Extracorporeal Photopheresis (ECP) used to treat it.
The various dressings used over the last four months have all needed to be kept dry, which has meant that I've only been able to get a shower when the dressings were due to be changed. Initially that was once per week, and later on twice per week, as changing the dressings too frequently (particularly in the early stages) impairs the healing process. As you might imagine, getting washed with a flannel on the other days has certainly given me a newfound appreciation for the inventor of showers!
Whilst the dressings do help to mask the sensitivity of the wounds, even wearing socks can still be slightly uncomfortable, as the stitching tends to be exactly where the wound is most sensitive. Having said that, what really made my big toes throb was if I didn't keep my feet elevated. It seemed like standing-up and walking around etc would make my big toes swell, and that resulted in the dressings applying more pressure.
It has only been in the last month or so that I've started to wear my trainers again, instead of the blue strap-on boots (see the photo below) provided by the hospital, as even though my big toes didn't look too bad after a couple of months, they were still quite sensitive, hence avoiding any pressure on them was far more comfortable. In fact, even now my big toes are still a little bit sensitive, but that should gradually fade over time as the skin hardens. Interestingly, once the skin has hardened, my big toes should be just as well-protected as when they had nails; Toenails don't really serve any purpose these days, so the only consequence of their removal is you have less to cut!
Fortunately, my big toes mostly feel fine now, albeit still slightly sensitive. As you no doubt noticed from the photos above, even after eighteen weeks, my big toes still have a small amount of healing left to do (more so on my right foot than my left foot), but I'm now really just hoping that the orthopedic surgeon managed to completely remove all traces of my big toenails, as I really don't want part of them to start growing back again. I'd like to be able to draw a line under the whole ingrowing toenails saga!
Sunday 30 March 2014
How do you know whether the ECP treatment is working?
It has been roughly a couple of months since I last mentioned how my skin GVHD is responding to ECP, and in that time I've had a further three treatments, bringing me to a grand total of twelve; The next is due to start in just over two weeks on the 15th of April (day +439). During that period, there have been some tweaks to how my skin GVHD is treated, but the real question is whether the ECP is actually working.
You may remember that after my tenth ECP treatment I was hoping to reduce their frequency from two-weekly to four-weekly. However, when that time came, the doctor instead decided to try reducing their frequency to three-weekly, whilst also reducing my Ciclosporin (immune suppressant) dose from 50mg/day to 25mg/day. The reason being that my skin GVHD didn't quite look under sufficient control to make the jump from two-weekly to four-weekly, hence splitting the difference made more sense. In addition, I was asked to apply Hydrocortisone cream for a week on the back of my hands, and for a few days around my mouth, as the skin GVHD was worst there.
After my eleventh ECP treatment, the doctor decided to continue as is, but to amend my use of creams, as my skin was quite dry, flaky and itchy, with varying degrees of discolouration/redness: I was prescribed Betnovate cream for use on my arms and legs as they were the worst affected areas, as well as some Diprobase cream to help moisturise all of my skin. The Betnovate cream is roughly one hundred times stronger than the Hydrocortisone cream, and the Diprobase cream consists of such a high percentage of paraffin that it comes with a warning that it will make you flammable! (I had been using Aqueous cream, but the Diprobase cream is a stronger moisturiser.)
Note: As you might imagine, frequently applying creams over nearly all of your body can become a somewhat tedious process. For that reason, combined with a mixture of laziness, a desire not to be a greasy, flammable mess, and past experience that my skin seemed to recover without using quite as much/strong of a cream as the doctors often prescribed, I decided to try only using the Betnovate cream initially, whilst also increasing my use of the Aqueous cream. My thinking was that it would be easy to see whether it was working or not, and I could always step things up if I needed to do so. As it turned-out, my skin improved quite quickly, and I even managed to reduce my use of the Betnovate cream a bit further, by sometimes using Aqueous cream instead.
After my twelfth ECP treatment, my skin was still slightly dry in places, but definitely better than three weeks prior, hence the doctor decided to try stopping my Ciclosporin (immune suppressant) altogether and reducing the frequency of my ECP treatments to four-weekly. As a result of the former, I could also stop taking my daily 5mg dose of Amlodipine, as it had originally been prescribed to help reduce my blood pressure, as the Ciclosporin had been making it a bit high. A week later, when having the routine blood tests and line flush, I asked the nurse to check my blood pressure, and it was was about 120 over 80, i.e. pretty much perfect. My pulse was still around 100bpm at rest though, which is a bit on the high side, and the most recent theory was that the Amlodipine was responsible for that, but it now seems like that's not the case.
Note: My twelfth ECP treatment was also my second three-monthly review, hence it was time for another lung function test, where I'd once again be complimented on my ability to breath normally, and a trip to the medication illustration department, where nearly all of my skin, as well as the inside of my mouth, would be photographed. I'm yet to hear the results of those, but I suspect the doctor will say they were fine.
Despite having had six months of ECP treatment now, it's still quite hard to say how much of a difference it alone is making to my skin GVHD. The reason being that the only way to even attempt to determine the answer to that question is to compare how my skin looked and felt six months ago with how it is today, whilst at the same time factoring in the changes that have been made in how the GVHD is being treated.
From my recollection, I would say that my skin itself is slightly worse than it was when I started the ECP treatment, as it looked and felt pretty much normal six months ago, due to the Ciclosporin (immune suppressant) and Prednisolone (steroid) medications working their magic, but it is slightly drier and flakier today. However, during that period, I have gradually reduced the medications, such that I've now stopped the Ciclosporin altogether and I'm taking precisely half of the dose of the Prednisolone. You can see exactly when and to what dose those medications were reduced, as well as when each of my ECP treatments started in the graph (and underlying tables) below:
From the above alone, you would likely conclude that the ECP treatment is making a difference, as even though my skin is slightly worse, the reduction in the medications is much more significant. However, for a couple of reasons, that's not really the whole picture. The first reason is that I would say that my skin is probably more similar now to how it was when I was only taking 20mg/day of Prednisolone, i.e. no Ciclosporin tablets or ECP treatments, hence in that respect the Ciclosporin is irrelevant. The second is that even though my Prednisolone dose is now precisely half of where I started, it hasn't been replaced by ECP alone, as I'm now frequently using Aqueous, Cetraben and Betnovate creams. (The latter being a quite strong topical steroid.)
In other words, once you take everything into account, I've essentially replaced the reduction in my Prednisolone dose with a combination of ECP and various creams. Unfortunately, that leaves the somewhat tricky question of how much the ECP and the various creams are individually contributing to the treatment of my skin GVHD. I did actually ask one of the doctors that very question, but it was clear from the smile and a slight shrugging of the shoulders that I got in response that no-one really knows. All I can say is that I have noticed that if I don't keep frequently applying the creams, it doesn't take all that long before my skin gradually starts to get worse, but at the same time it does seem like it takes longer now than before I started the ECP treatment.
The Tweaks
You may remember that after my tenth ECP treatment I was hoping to reduce their frequency from two-weekly to four-weekly. However, when that time came, the doctor instead decided to try reducing their frequency to three-weekly, whilst also reducing my Ciclosporin (immune suppressant) dose from 50mg/day to 25mg/day. The reason being that my skin GVHD didn't quite look under sufficient control to make the jump from two-weekly to four-weekly, hence splitting the difference made more sense. In addition, I was asked to apply Hydrocortisone cream for a week on the back of my hands, and for a few days around my mouth, as the skin GVHD was worst there.
After my eleventh ECP treatment, the doctor decided to continue as is, but to amend my use of creams, as my skin was quite dry, flaky and itchy, with varying degrees of discolouration/redness: I was prescribed Betnovate cream for use on my arms and legs as they were the worst affected areas, as well as some Diprobase cream to help moisturise all of my skin. The Betnovate cream is roughly one hundred times stronger than the Hydrocortisone cream, and the Diprobase cream consists of such a high percentage of paraffin that it comes with a warning that it will make you flammable! (I had been using Aqueous cream, but the Diprobase cream is a stronger moisturiser.)
Note: As you might imagine, frequently applying creams over nearly all of your body can become a somewhat tedious process. For that reason, combined with a mixture of laziness, a desire not to be a greasy, flammable mess, and past experience that my skin seemed to recover without using quite as much/strong of a cream as the doctors often prescribed, I decided to try only using the Betnovate cream initially, whilst also increasing my use of the Aqueous cream. My thinking was that it would be easy to see whether it was working or not, and I could always step things up if I needed to do so. As it turned-out, my skin improved quite quickly, and I even managed to reduce my use of the Betnovate cream a bit further, by sometimes using Aqueous cream instead.
After my twelfth ECP treatment, my skin was still slightly dry in places, but definitely better than three weeks prior, hence the doctor decided to try stopping my Ciclosporin (immune suppressant) altogether and reducing the frequency of my ECP treatments to four-weekly. As a result of the former, I could also stop taking my daily 5mg dose of Amlodipine, as it had originally been prescribed to help reduce my blood pressure, as the Ciclosporin had been making it a bit high. A week later, when having the routine blood tests and line flush, I asked the nurse to check my blood pressure, and it was was about 120 over 80, i.e. pretty much perfect. My pulse was still around 100bpm at rest though, which is a bit on the high side, and the most recent theory was that the Amlodipine was responsible for that, but it now seems like that's not the case.
Note: My twelfth ECP treatment was also my second three-monthly review, hence it was time for another lung function test, where I'd once again be complimented on my ability to breath normally, and a trip to the medication illustration department, where nearly all of my skin, as well as the inside of my mouth, would be photographed. I'm yet to hear the results of those, but I suspect the doctor will say they were fine.
The Real Question
Despite having had six months of ECP treatment now, it's still quite hard to say how much of a difference it alone is making to my skin GVHD. The reason being that the only way to even attempt to determine the answer to that question is to compare how my skin looked and felt six months ago with how it is today, whilst at the same time factoring in the changes that have been made in how the GVHD is being treated.
From my recollection, I would say that my skin itself is slightly worse than it was when I started the ECP treatment, as it looked and felt pretty much normal six months ago, due to the Ciclosporin (immune suppressant) and Prednisolone (steroid) medications working their magic, but it is slightly drier and flakier today. However, during that period, I have gradually reduced the medications, such that I've now stopped the Ciclosporin altogether and I'm taking precisely half of the dose of the Prednisolone. You can see exactly when and to what dose those medications were reduced, as well as when each of my ECP treatments started in the graph (and underlying tables) below:
From the above alone, you would likely conclude that the ECP treatment is making a difference, as even though my skin is slightly worse, the reduction in the medications is much more significant. However, for a couple of reasons, that's not really the whole picture. The first reason is that I would say that my skin is probably more similar now to how it was when I was only taking 20mg/day of Prednisolone, i.e. no Ciclosporin tablets or ECP treatments, hence in that respect the Ciclosporin is irrelevant. The second is that even though my Prednisolone dose is now precisely half of where I started, it hasn't been replaced by ECP alone, as I'm now frequently using Aqueous, Cetraben and Betnovate creams. (The latter being a quite strong topical steroid.)
In other words, once you take everything into account, I've essentially replaced the reduction in my Prednisolone dose with a combination of ECP and various creams. Unfortunately, that leaves the somewhat tricky question of how much the ECP and the various creams are individually contributing to the treatment of my skin GVHD. I did actually ask one of the doctors that very question, but it was clear from the smile and a slight shrugging of the shoulders that I got in response that no-one really knows. All I can say is that I have noticed that if I don't keep frequently applying the creams, it doesn't take all that long before my skin gradually starts to get worse, but at the same time it does seem like it takes longer now than before I started the ECP treatment.
Friday 28 February 2014
The hidden scars of cancer treatment
For many cancer survivors, particularly those that had hematological malignancies, if you were to bump in to them at the beach, you would likely never know what their bodies had been put through. The reason being that often the treatment only involves chemotherapy, radiotherapy and/or stem cell transplants, hence any damage caused in the process is likely well-hidden beneath the skin. For that reason, this post is about the hidden scars that I've acquired on my now five-year journey of cancer treatment.
As it happens, my timing of this post is not ideal, as I need to start by contradicting myself a little. Due to my recent toenail surgery, hickman line replacement, and skin GVHD issues, I do actually have more visible on the surface than usual, so even the least observant amongst you would likely notice something. However, the first two will shortly be not so easy to spot (given sufficient time to heal), and the dry, flaky, red skin caused by the last (should it not be cured) might easily be mistaken for soaking-up too many of the sun's rays. Having said that, if you were to put your detective hat on, and look at me closely, there are a few things that you couldn't dismiss as normal:
Finally wrapping this post up, hopefully the extensive albeit still incomplete description above gives you an appreciation for what I now consider to be my new normal; Hence, if you do ever bump in to me at the beach one day, and ask how I'm doing and say that I look well, you will know why I smile when replying: "I'm fine, thanks. How are you?"
As it happens, my timing of this post is not ideal, as I need to start by contradicting myself a little. Due to my recent toenail surgery, hickman line replacement, and skin GVHD issues, I do actually have more visible on the surface than usual, so even the least observant amongst you would likely notice something. However, the first two will shortly be not so easy to spot (given sufficient time to heal), and the dry, flaky, red skin caused by the last (should it not be cured) might easily be mistaken for soaking-up too many of the sun's rays. Having said that, if you were to put your detective hat on, and look at me closely, there are a few things that you couldn't dismiss as normal:
-
Scars - There are several very minor scars, which are only just visible upon close inspection, as a result of having a number of bone marrow and skin biopsies, and hickman line insertions and removals.
-
Tattoos - There are a few tiny tattoos, which are simply dots of about one millimetre diameter, that were used in the targeting of the radiotherapy.
-
Missing Toenails - The nails on my big toes are missing, due to them being permanently removed to prevent an infection from reoccurring.
-
Hearing Difficulties - One of the chemotherapy drugs that I had during my second-line treatment, namely Cisplatin, damaged my hearing in a couple of ways. The damage consists of Tinnitus (a constant ringing sound) and loss of high frequencies; It is worse in my left ear. Whilst I don't notice it most of the time, as my idea of normal has gradually changed, I do struggle to pick-out voices in busier/noisier environments; Background noises, such as fans humming or numerous distant conversations, have a tendency to drowned-out nearby voices, especially women's voices.
-
Hair Loss - A number of the treatments have caused my hair to fall out, and whilst in the early days it eventually grew back, it is a lot thinner these days, hence being bald (or having really short hair) is about the only style that I can manage now, without giving away that something isn't quite right. Fortunately, I'm used to having short hair, so it doesn't bother me. In fact, I actually wish that it wouldn't grow at all, as it would be easier that way.
-
Scar Tissue - Despite the cancerous masses shrinking substantially as a result of the treatments I've had, there is still a significant amount of scar tissue left behind; It's similar to how if you inflate a balloon, and then let all of the air out, the balloon doesn't go back to its original size and shape. This doesn't pose a problem for myself, in that I can't tell that it's there, but it does complicate the interpretation of any medical imaging, as it can be hard to differentiate innocuous scar tissue from cancerous masses.
-
Weight Changes - The cancer and its treatment has caused my weight to drop overall, but not in a good way. Unfortunately, when your body is going through such a process, it is the lean muscle mass that it burns for its additional requirements. Also, even though you may be given steroids as part of your medications, which can dramatically increase your appetite, the type of steroids you're likely to be given (corticosteroids) don't help, as they often cause a redistribution of body fat to the face and torso, and with long-term use can lead to muscle wasting. (It's anabolic steroids that are used in bodybuilding, i.e. corticosteroids can have the opposite effect.)
-
Infertility - Most of the treatments affect fertility; For some it's likely to be a temporary side effect, but for others it's likely permanent. Whilst I've not actually been tested myself, it seems very unlikely that I will be fertile after all of the treatments that I've had. Fortunately, there are options such as adoption, should I ever want children, hence it is not a big issue for me.
-
Lung Damage - By comparing the results of my first and last lung function tests, you can see that my lungs have suffered from friendly-fire at times, as they don't work as well as they used to do. I'm only likely to notice the damage when my lungs have to work harder though, e.g. when exercising.
-
Peripheral Sensory Neuropathy - The monoclonal antibody-drug conjugate that I had during my third-line treatment, namely Brentuximab Vedotin, damaged the nerves in the extremities of my hands and feet. It's mostly my finger tips where I notice it now, as they often feel numb, tingly and tender. My fingers do tremble slightly at times now too, especially when performing tasks that require any precision or a light touch.
Finally wrapping this post up, hopefully the extensive albeit still incomplete description above gives you an appreciation for what I now consider to be my new normal; Hence, if you do ever bump in to me at the beach one day, and ask how I'm doing and say that I look well, you will know why I smile when replying: "I'm fine, thanks. How are you?"
Saturday 1 February 2014
How was the hickman line issue resolved?
During the eighth ECP treatment was when an issue with my hickman line was discovered, but, to quote one of the nurses, despite trying me in more positions than in the Kama Sutra, drawing blood from it was still far more 'miss' than 'hit'. The rationale behind waving my arms around, turning my head, laying down, taking deep breaths, coughing and so on was that sometimes the hickman line can get into a position where it's problematic for drawing blood, hence by taking such actions things can move around a little, which may result in the hickman line starting to work.
Note: If you imagine the hole(s) in the hickman line being close to/up against a vein, the sucking action of trying to draw blood can result in those hole(s) being plugged with the wall of the vein, thereby preventing any blood from being withdrawn.
Another issue that can occur is that the hickman line can become blocked, as a result of blood clots, either within the hickman line itself or at the entry/exit points in the vein. When there is suspicion that a hickman line might be blocked, a small amount of Urokinase can be pushed in, and left there for (at least) forty-five minutes. The Urokinase is pretty much the hickman line equivalent of a drain cleaner, in that it hopefully breaks-up/dissolves any blood clots, thereby unblocking the hickman line.
In my case, there were no issues with pushing fluids in, hence it likely wasn't blocked within the hickman line itself, but it could potentially be blocked at the entry/exit points, as sometimes the blood clots over the hole(s) in the hickman line and acts like a one-way valve, i.e. pushing fluids in opens the valve, but trying to pull fluids out closes it. In some ways, it's very similar to how the wall of a vein can act like a plug.
Note: Trying to push/pull any fluids in/out of the hickman line can often be enough by itself to clear any blockages, as the pressure caused by doing so is sufficient to dislodge them; That's why a few techniques of applying sharper bursts of pressure than usual (due to concerns of causing damage) are sometimes attempted.
Unfortunately, despite a few attempts at using Urokinase etc, my hickman line still only worked intermittently at best, hence the next step was to go for a lineogram. A lineogram essentially involves the use of contrast fluid and x-rays to check the positioning of, and see what is happening with, the hickman line. If the hickman line needs repositioning, it is sometimes possible to do so, but it tends to depend on how long it has been in, as after so long they are pretty much stuck in place. If the hickman line needs unblocking, it is sometimes possible to use a thin wire to clear any blood clots that the Urokinase was unable to break-up/dissolve. If all else fails, then the only option remaining is to remove the old hickman line and insert a new one.
When I had my lineogram, all of the preparation for replacing the hickman line also took place (just in case), i.e. surgical sheets were positioned as necessary, the area where the hickman line would be removed and inserted was cleaned with an alcohol solution, and so on. It should have occurred to me really, but the combination of dry skin, caused by GVHD, and alcohol solution, for cleaning it, is the perfect recipe for some pretty unpleasant burning/stinging sensations! After that, any local anesthetic would have seemed like a walk in the park. Fortunately, even though my chest and neck felt like it was on fire, the thin wire managed to unblock my hickman line, so I didn't actually need to have it replaced. Having said that, a few hours later, when a nurse tried to take some blood samples from it, it was back to its intermittent ways! Unfortunately, that meant the old hickman line coming out, and a new one going in. However, it was Christmas Eve, so that pleasure was saved for another day.
The timing of my lineogram actually reminds me of an amusing story. As is often the case in hospital rooms with imaging devices, there was air conditioning to prevent the equipment from over-heating, and that meant it felt pretty cold in there, especially as I had to wear one of those thin hospital gowns. Consequently, whilst waiting for the lineogram to begin, I was wrapped-up in some blankets to help keep me warm. One of those blankets was a space blanket, i.e. what looks like a large piece of tinfoil. As you might imagine, it wasn't long after being wrapped-up in the space blanket before I was being compared to a Christmas turkey. All I had to say was: I'm not sure how many x-rays it takes to cook a Christmas turkey, but if I see anyone come anywhere near me with sage and onion stuffing, I'll be out of here quicker than you can say Paxo!
On New Year's Eve, I had my old hickman line removed, which was nothing to worry about really; I only felt some burning/stinging sensations from the alcohol solution and local anesthetic, even though the doctor did have some fun with a scalpel trying to remove the well knitted-in cuff (designed to hold the hickman line in place). A couple of days later, a new hickman line was inserted, which was also a non-event really, even though it also meant yet more burning/stinging sensations from the alcohol solution and local anesthetic. The end result was that my chest and neck was decorated with dressings, as you can see in the photo below (click on the photo to see it full size):
Note: If you imagine the hole(s) in the hickman line being close to/up against a vein, the sucking action of trying to draw blood can result in those hole(s) being plugged with the wall of the vein, thereby preventing any blood from being withdrawn.
Another issue that can occur is that the hickman line can become blocked, as a result of blood clots, either within the hickman line itself or at the entry/exit points in the vein. When there is suspicion that a hickman line might be blocked, a small amount of Urokinase can be pushed in, and left there for (at least) forty-five minutes. The Urokinase is pretty much the hickman line equivalent of a drain cleaner, in that it hopefully breaks-up/dissolves any blood clots, thereby unblocking the hickman line.
In my case, there were no issues with pushing fluids in, hence it likely wasn't blocked within the hickman line itself, but it could potentially be blocked at the entry/exit points, as sometimes the blood clots over the hole(s) in the hickman line and acts like a one-way valve, i.e. pushing fluids in opens the valve, but trying to pull fluids out closes it. In some ways, it's very similar to how the wall of a vein can act like a plug.
Note: Trying to push/pull any fluids in/out of the hickman line can often be enough by itself to clear any blockages, as the pressure caused by doing so is sufficient to dislodge them; That's why a few techniques of applying sharper bursts of pressure than usual (due to concerns of causing damage) are sometimes attempted.
Unfortunately, despite a few attempts at using Urokinase etc, my hickman line still only worked intermittently at best, hence the next step was to go for a lineogram. A lineogram essentially involves the use of contrast fluid and x-rays to check the positioning of, and see what is happening with, the hickman line. If the hickman line needs repositioning, it is sometimes possible to do so, but it tends to depend on how long it has been in, as after so long they are pretty much stuck in place. If the hickman line needs unblocking, it is sometimes possible to use a thin wire to clear any blood clots that the Urokinase was unable to break-up/dissolve. If all else fails, then the only option remaining is to remove the old hickman line and insert a new one.
When I had my lineogram, all of the preparation for replacing the hickman line also took place (just in case), i.e. surgical sheets were positioned as necessary, the area where the hickman line would be removed and inserted was cleaned with an alcohol solution, and so on. It should have occurred to me really, but the combination of dry skin, caused by GVHD, and alcohol solution, for cleaning it, is the perfect recipe for some pretty unpleasant burning/stinging sensations! After that, any local anesthetic would have seemed like a walk in the park. Fortunately, even though my chest and neck felt like it was on fire, the thin wire managed to unblock my hickman line, so I didn't actually need to have it replaced. Having said that, a few hours later, when a nurse tried to take some blood samples from it, it was back to its intermittent ways! Unfortunately, that meant the old hickman line coming out, and a new one going in. However, it was Christmas Eve, so that pleasure was saved for another day.
The timing of my lineogram actually reminds me of an amusing story. As is often the case in hospital rooms with imaging devices, there was air conditioning to prevent the equipment from over-heating, and that meant it felt pretty cold in there, especially as I had to wear one of those thin hospital gowns. Consequently, whilst waiting for the lineogram to begin, I was wrapped-up in some blankets to help keep me warm. One of those blankets was a space blanket, i.e. what looks like a large piece of tinfoil. As you might imagine, it wasn't long after being wrapped-up in the space blanket before I was being compared to a Christmas turkey. All I had to say was: I'm not sure how many x-rays it takes to cook a Christmas turkey, but if I see anyone come anywhere near me with sage and onion stuffing, I'll be out of here quicker than you can say Paxo!
On New Year's Eve, I had my old hickman line removed, which was nothing to worry about really; I only felt some burning/stinging sensations from the alcohol solution and local anesthetic, even though the doctor did have some fun with a scalpel trying to remove the well knitted-in cuff (designed to hold the hickman line in place). A couple of days later, a new hickman line was inserted, which was also a non-event really, even though it also meant yet more burning/stinging sensations from the alcohol solution and local anesthetic. The end result was that my chest and neck was decorated with dressings, as you can see in the photo below (click on the photo to see it full size):
Monday 27 January 2014
When do you try tapering-off the ECP treatment?
Since October, my care seems to have mostly focused on treating infections, i.e. the Hodgkin's Lymphoma and skin GVHD has almost seemed incidental. That's not too surprising though really, given that between October and December I spent over half of my time as an inpatient on IV antibiotics. However, in the background, the fortnightly ECP treatments at Rotherham General Hospital still needed to take place, hence I've continued with regularly zapping those white blood cells of mine with UV light.
I've actually had nine ECP treatments now, and it's still proving to be an easy ride, as I've not had any noticeable side effects really. Having said that, there have been some bumps in the road. As you can likely appreciate, I've been unable to beat my record for the walking test, as my big toes have been quite sore at times, hence I've skipped the walking test, as seeing how far I could hobble along the hospital corridors would have been a meaningless exercise really. Also, in late December, my hickman line decided that it was no longer willing to part with my blood, and that resulted in my eighth ECP treatment being delayed by three weeks, whilst I could get my hickman line sorted.
Despite my first attempt at the eighth ECP treatment failing on both days, leading to it eventually being rescheduled for three weeks later, the first day wasn't an entirely wasted journey, as I did still go to the medical illustration department, where another set of photos of my skin were taken for comparison purposes; i.e. another member of the NHS staff had the misfortune/pleasure of me flashing my bum at them. Another lung function test was also necessary for comparison purposes, but that never took place until I had my ninth ECP treatment, as that required an appointment to be made; Once again, I was congratulated (a few times) on my ability to breath normally.
My hickman line playing-up did complicate my ECP treatment schedule, as instead of there being two weeks between my seventh and eighth ECP treatments, there was actually five weeks. As you may remember, after the eighth ECP treatment is when my progress needed reviewing, in order to determine whether the ECP treatments seemed to be working, and consequently whether their frequency needed adjusting. That review did take place, albeit three weeks later than planned, and it was decided that my ninth ECP treatment should be only two weeks after the eighth, and then I should switch to every four weeks, as that would pretty much bring me back on track.
Note: My Prednisolone (steroid) dose was reduced from essentially 12.5mg/day to 10mg/day after my fifth ECP treatment, and my Ciclosporin (immune suppressant) dose was reduced from 75mg/day to 50mg/day after my eighth ECP treatment, hence the doses of those medications were (and still are) at most half of where I started.
Unfortunately, after my ninth ECP treatment, those plans were changed, as it was decided that my tenth ECP treatment should be two (not four) weeks later, due to my skin being pretty dry in numerous places, looking slightly discoloured on my arms and legs, and appearing especially red on the back of my hands. To be fair, judging my progress with the ECP treatments isn't exactly easy, as there are a few potential causes of my skin GVHD flaring-up, i.e. it's hard to know what is causing what.
Note: The infections that I've had recently will have caused my immune system to ramp-up, which can result in flare-ups of GVHD, i.e. my skin may have been caught in the cross-fire. Also, I haven't been able to get a shower as often as normal, which is when I usually applied the moisturising cream to help protect my skin; The dressings on my big toes, from having my toenails surgically removed, and on my chest and neck, from getting my hickman line sorted, has meant that I've often just been getting a wash, rather than a shower, due to having to keep the dressings dry unless they were about to be changed. Finally, the ECP treatments may not be working sufficiently well to counteract the reduction in the steroid and immune suppressant doses.
Hopefully, after the tenth ECP treatment, I will be able to switch to only returning every four weeks, but given that it's still a little over a week away at this point, only time will tell whether that proves to be the case. However, in the mean time, I will leave you with a photo of some pretty neat art on the Rotherham General Hospital roof - I can't help but notice it, as I hobble my way along the corridor to the ECP treatment room:
I've actually had nine ECP treatments now, and it's still proving to be an easy ride, as I've not had any noticeable side effects really. Having said that, there have been some bumps in the road. As you can likely appreciate, I've been unable to beat my record for the walking test, as my big toes have been quite sore at times, hence I've skipped the walking test, as seeing how far I could hobble along the hospital corridors would have been a meaningless exercise really. Also, in late December, my hickman line decided that it was no longer willing to part with my blood, and that resulted in my eighth ECP treatment being delayed by three weeks, whilst I could get my hickman line sorted.
Despite my first attempt at the eighth ECP treatment failing on both days, leading to it eventually being rescheduled for three weeks later, the first day wasn't an entirely wasted journey, as I did still go to the medical illustration department, where another set of photos of my skin were taken for comparison purposes; i.e. another member of the NHS staff had the misfortune/pleasure of me flashing my bum at them. Another lung function test was also necessary for comparison purposes, but that never took place until I had my ninth ECP treatment, as that required an appointment to be made; Once again, I was congratulated (a few times) on my ability to breath normally.
My hickman line playing-up did complicate my ECP treatment schedule, as instead of there being two weeks between my seventh and eighth ECP treatments, there was actually five weeks. As you may remember, after the eighth ECP treatment is when my progress needed reviewing, in order to determine whether the ECP treatments seemed to be working, and consequently whether their frequency needed adjusting. That review did take place, albeit three weeks later than planned, and it was decided that my ninth ECP treatment should be only two weeks after the eighth, and then I should switch to every four weeks, as that would pretty much bring me back on track.
Note: My Prednisolone (steroid) dose was reduced from essentially 12.5mg/day to 10mg/day after my fifth ECP treatment, and my Ciclosporin (immune suppressant) dose was reduced from 75mg/day to 50mg/day after my eighth ECP treatment, hence the doses of those medications were (and still are) at most half of where I started.
Unfortunately, after my ninth ECP treatment, those plans were changed, as it was decided that my tenth ECP treatment should be two (not four) weeks later, due to my skin being pretty dry in numerous places, looking slightly discoloured on my arms and legs, and appearing especially red on the back of my hands. To be fair, judging my progress with the ECP treatments isn't exactly easy, as there are a few potential causes of my skin GVHD flaring-up, i.e. it's hard to know what is causing what.
Note: The infections that I've had recently will have caused my immune system to ramp-up, which can result in flare-ups of GVHD, i.e. my skin may have been caught in the cross-fire. Also, I haven't been able to get a shower as often as normal, which is when I usually applied the moisturising cream to help protect my skin; The dressings on my big toes, from having my toenails surgically removed, and on my chest and neck, from getting my hickman line sorted, has meant that I've often just been getting a wash, rather than a shower, due to having to keep the dressings dry unless they were about to be changed. Finally, the ECP treatments may not be working sufficiently well to counteract the reduction in the steroid and immune suppressant doses.
Hopefully, after the tenth ECP treatment, I will be able to switch to only returning every four weeks, but given that it's still a little over a week away at this point, only time will tell whether that proves to be the case. However, in the mean time, I will leave you with a photo of some pretty neat art on the Rotherham General Hospital roof - I can't help but notice it, as I hobble my way along the corridor to the ECP treatment room:
Subscribe to:
Posts (Atom)