You may not realise this, but chemotherapy is really just a general term for a type of cancer treatment, so when different people say that they have had chemotherapy it is entirely possible that they have had completely different drugs to one and other. There are about sixty different individual chemotherapy drugs, and regimens are typically made up of a few of them, hence there are quite a number of possible combinations; However, in reality there is a much smaller number of regimens than theoretically possible - Coincidentally, there are also about sixty. The different regimens are used for different types of cancer, but factors such as your medical history also come into it.
Note: The individual chemotherapy drug and regimen statistics are based on counting those currently listed by Macmillan Cancer Support, and their lists are not exhaustive, but even so they do help to illustrate the point that chemotherapy is not just one drug.
The chemotherapy that I am having for this particular treatment is a regimen called IVE, which contains three chemotherapy drugs: Ifosfamide, Epirubicin and Etoposide. If you were to read the list of possible side effects of those chemotherapy drugs, you would likely be looking for the nearest emergency exit. Fortunately, there are medications that help alleviate some of the side effects (most notably, anti-sickness drugs); However, as much as they might help, it is still likely to be an unpleasant experience - The reason I say likely is that the side effects do vary from one person to the next, both in terms of what side effects they get, as well as their intensity.
The previous times that I was treated for Hodgkin's Lymphoma I had always had different chemotherapy regimens, and although one of those regimens did include Etoposide I still didn't really know what exactly to expect, as when taken with different chemotherapy drugs the side effects do vary; Obviously I had some idea, but I also knew that each of the regimens I'd had up until then had affected me differently. All of the chemotherapy drugs that I needed for this regimen were administered intravenously (via IV) - In other words, dripped/injected directly into the blood stream.
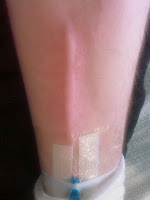
The first chemotherapy drug that I had in this regimen was Epirubicin, which involved two syringes of a red coloured fluid being slowly injected (each over five or so minutes) into a cannula in my arm. However, this did not exactly go smoothly, as the small veins in my arm did not take too kindly to the experience: about halfway through the first syringe the veins in my arm started to swell-up quite a lot, due to an irritation/reaction - The nurse finished the syringe really slowly, but then had to stop to seek advice about how to proceed; It appears the irritation/reaction was unusual, as a number of nurses were curious and came to have a look before a doctor looked and decided that I would need a femoral line inserting for the remainder of my chemotherapy - The reason being that the femoral line goes into a much bigger vein, and when combined with a drug to help prevent reactions the remainder of the chemotherapy should be problem free. In case you are curious, here are a few pictures I took:
The remainder of the Epirubicin was injected into the femoral line, and that went fine, so other than the Epirubicin making my urine turn red for a bit, I couldn't really attribute anything else to it for certain. Next up was the Etoposide, which came in two one litre bags, each of which takes an hour to drip through; by the end of the two hours, I was starting to feel really nauseous. Finally, or so I thought at the time, was the Ifosfamide, which came in three one litre bags, each of which takes seven hours to drip through - A drug called Mesna is also administered at the same time, as the Ifosfamide can irritate the bladder: the Mesna helps to prevent the irritation from happening. The nausea seemed to lessen whilst the Ifosfamide was administered, which was definitely welcomed. To my surprise though, I now had a further two doses of both the Etoposide and Ifosfamide, hence another couple of days went by before it was all finally wrapped-up with a litre of Mesna, which took twelve hours to drip through. During this period, the level of nausea was up and down a fair bit, and I was sick too, which is never a pleasant experience even if you do feel a bit better afterwards. I also felt quite tired at times, probably due to the chemotherapy, but also because it can be quite hard to sleep in the hospital, as mattresses aside the nurses need to regularly check your blood pressure, temperature, pulse and oxygen saturation, as well as disconnect and connect the different chemotherapy drugs. The only other noticeable side effect was loss of appetite; I lost over half a stone in a few days.
In total it took around five days to complete the IVE chemotherapy, and I got to go home pretty much straight afterwards - The femoral line had to be removed before I could go home. That meant I had a couple of weeks or so to recover before the next session of chemotherapy. In that couple of weeks, I just had to: come back after about a week for a check-up, i.e. to have a blood test and to talk to a doctor about how I was getting on; and shortly before the next treatment go to get a hickman line inserted, which would hopefully be used for the rest of my treatment, and make things easier. If you could see all of the bruises on my forearms after just a week of blood tests and treatment, you would fully understand why I say that - I've not taken a picture, as we all know what bruises look like!
When discharged from the hospital, I was given a bunch of medications: Ondansetron (anti-sickness), Co-trimoxazole (anti-bacterial), Aciclovir (anti-viral) and Fluconazole (anti-fungal) being those that are typically prescribed. Also, because this was my first session of chemotherapy in this round of treatment, I was also given some Allopurinol tablets to help my kidneys with the side effects of the chemotherapy. If that wasn't enough, I was also given a week's worth of Filgrastim (G-CSF) injections to help boost my immune system, as the chemotherapy pretty much kicked its ass! You may now understand why I have to take all of those tablets for fighting infections - My immune system is essentially compromised, so infections that it would normally just handle without any real fuss can now be a much bigger deal. This is also the reason that it is recommended to avoid certain foods, as well as takeaways, and just to generally be extra vigilant about hygiene.
All of the medications and injections are no problem really, but I must admit I do always hesitate a little before injecting myself in the stomach - It's not that it particularly hurts or anything; It's just the idea of putting a needle in to my stomach makes me stop and think a bit. The only thing that is worth mentioning about the injections is that you do sometimes start to feel them kick-in: you feel a kind of pulsing pain in the centre of your lower back. With the Filgrastim injections, it has never really been that bad for me, perhaps because they are lower doses over a number of days, but I have also had Pegfilgrastim, which I assume is essentially just a single larger dose, and then the pain has been really bad; Patients have been known to go into accident and emergency departments with it, and despite being given strong pain-killers such as morphine not feel any better - Surprisingly, paracetamol is actually really effective though, which you would likely never even consider if you felt it yourself. The pain seems to be triggered by moving, and it does ease dramatically if you stay still, but it is not that easy to stay still, as it really does hurt, and your instincts are telling you to move. It did once kick-in whilst I was visiting one of my cousins, and I think she was pretty worried, as she could see how much it hurt - I could hardly breath let alone speak as she carefully drove me home! Once I laid down on my bed, after taking some paracetamol, I felt much better after half an hour or so.
At home, after the IVE chemotherapy, I still felt nauseous, and I was a bit tired, but it was more that I was easily out of breath than anything; for example, the next morning after a few minutes in the shower, I had no choice but to sit down, as it felt like I was about to pass out. I apparently looked pretty shocking too, as there was a lot of black around my eyes. However, over the next few days, I gradually improved and was eating and drinking a lot better. It was probably about five days though before I could simply stand still for more than a few minutes without feeling exhausted and needing to sit down. The next day, things didn't go so smoothly though, but that's a story for another post...


No comments:
Post a Comment